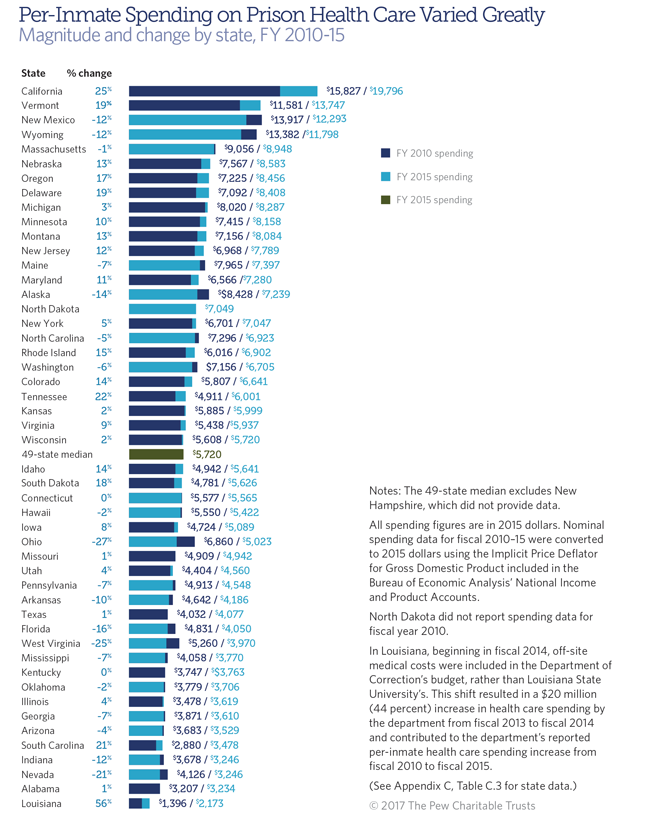
Prison Health Care Spending Varies Dramatically by State
Why such a discrepancy, and what does it indicate?
This is the fourth analysis in a series examining how health care is funded and delivered in state-run prisons, as well as how care continuity is facilitated upon release.
Every state has an interest in delivering health care in its prisons that conforms to constitutional requirements and leverages opportunities to improve public health and reduce crime and recidivism. Nevertheless, the provision of care throughout the country varies significantly. There is no starker evidence of this dissimilarity than the wide range in what states spend per inmate. (See graphic below.)
What drives these dramatic differences? To what extent do they reflect meaningful discrepancies in value and performance that move some states closer to reaching their common ends, while pushing others further away? The answers to these questions provide critical information for any assessment of whether states are doing all they can to protect their communities, strengthen public health, and spend money wisely.
Persistent per-inmate spending variation
In fiscal year 2015, the typical state department of corrections spent $5,720 per inmate to provide health care services, including medical, dental, mental health, and substance use treatment. However, departments in four states (California, New Mexico,1 Vermont, and Wyoming) spent more than $10,000 per inmate, while five (Alabama, Indiana, Louisiana, Nevada, and South Carolina) spent less than $3,500 per inmate. This ordering and breadth of variation tracked closely with prior years.
Note: For state data and data notes, see Figure 2 and Appendix C, Table C.3 of “Prison Health Care: Costs and Quality.”
Variation drivers
The Bureau of Justice Statistics has pointed to several factors that possibly contribute to state-to-state spending differences, including pre-incarceration care, regional medical prices, staffing and compensation levels, facility capacity and related fixed costs or bulk purchasing, and incidences of high-risk behaviors and associated disease burdens. Other researchers have examined additional reasons, including contracting practices, screening procedures, and cost-containment strategies.
Crucially, studies have omitted two variables critical to any complete evaluation of spending: access to care and quality of care. This is probably because of the lack of uniform quality-of-care standards and reporting for correctional systems, which would permit more complete comparisons across states and facilities. Little has been known systematically about states’ quality monitoring activities and actual outcomes.
Pew research examines spending variation
A first-of-its-kind report by The Pew Charitable Trusts explores several factors behind interstate spending variation, such as how money is spent, prices prisons pay, the people they treat, and the quality of care provided. The report highlights some of the main data officials need to determine what outcomes are achieved with prison health care dollars, and to map out avenues for any necessary changes. Information is provided on:
- Spending distributions. Beyond topline spending data, officials benefit from actionable, disaggregated figures, which can be used to understand per-inmate expenditure variation, evaluate the cost-effectiveness of care, and better manage systems. Still, many states report having a limited ability to dig deep into spending data, commonly citing as barriers systems that do not allow for such parsing or a lack of access to records from contractors.
- Staffing. States reported dramatically different approaches to staffing by departments of corrections and their vendor and university partners in fiscal 2015. Not surprisingly, staffing levels appear to correlate with per-inmate prison health care expenditures: Median per-inmate spending was more than double among the 10 states with the highest staffing levels than the 10 states with the lowest levels.
- Patient characteristics. The composition of individuals covered can have a dramatic effect on costs for any health care payer, including prisons. Key interrelated predictors include age, sex, and health status. Unfortunately, comparable disease burden data are not available state by state for incarcerated individuals, in part because of the absence of regular reporting and inconsistency in prevalence tracking practices. However, some insights are gleaned from examining the presence of older individuals and women. Both cohorts are disproportionately likely to report a current or past chronic condition, and rates of mental illness among women in prison are substantially higher than average, in part because of high rates of childhood sexual abuse and post-traumatic stress disorder.
- Care quality. The nature of the health care that prisons provide affects individuals’ well-being and whether states are able to cost-effectively and sustainably meet their objectives. Nevertheless, policymakers and administrators do not always have the information they need—or regularly use what they do have—to proactively identify shortcomings and make improvements. Thirty-five states reported that they operated a prison health care quality monitoring system in fiscal 2016, though these varied significantly with respect to objectives, scope, focus, and whether and how they were used to inform spending and management decisions.
In some cases, states lack the information necessary to fully understand what they are getting for their prison health care dollars or have not taken important steps to cement their processes and act upon the data. Moreover, much of what does exist lacks the level of uniformity and standardization necessary to appropriately make state-to-state comparisons.
Higher spending is not necessarily an indication of either waste or good quality care. Likewise, lower spending is not necessarily a sign of efficiency or poor quality. Instead, policymakers must seek to continually appraise the value their systems achieve.
Matt McKillop is an officer with the states’ fiscal health project of The Pew Charitable Trusts.
- On Oct. 27, 2017, the New Mexico Corrections Department (NMCD) reported to Pew researchers that its per-inmate health care spending figures in this report are inaccurate, reflecting incorrect information provided earlier by department officials. Pew has asked the state to supply in writing revised data and guidance; once these are submitted, Pew will amend or update the report as necessary. Questions related to these data should be directed to NMCD.
Spotlight on Mental Health
MORE FROM PEW
Explore Pew’s new and improved
Fiscal 50 interactive
Your state's stats are more accessible than ever with our new and improved Fiscal 50 interactive:
- Maps, trends, and customizable charts
- 50-state rankings
- Analysis of what it all means
- Shareable graphics and downloadable data
- Proven fiscal policy strategies
Welcome to the new Fiscal 50
Key changes include:
- State pages that help you keep track of trends in your home state and provide national and regional context.
- Interactive indicator pages with highly customizable and shareable data visualizations.
- A Budget Threads feature that offers Pew’s read on the latest state fiscal news.