A Combination of Approaches Helps Local Governments Tackle the Opioid Crisis
9 key takeaways from Philadelphia, Baltimore, Staten Island, and beyond
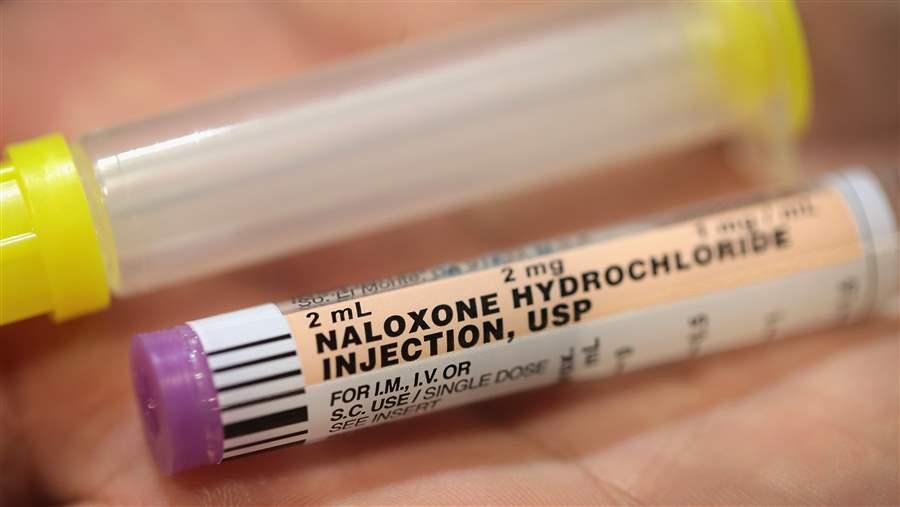
Naloxone is a prescription drug that can reverse the effects of an opioid overdose.
Scott Olson/Getty ImagesThe Pew Charitable Trusts recently hosted a panel discussion in Philadelphia on how the city and other urban areas, such as Baltimore and Staten Island, New York, are responding to the opioid crisis. Focusing on the latest evidence-based strategies for improving treatment and prevention, the April 20 event highlighted innovative, multifaceted responses that have been successful in all three jurisdictions and elsewhere.
Here are nine policies and practices highlighted by the panelists—Evan Behrle, special adviser on opioid policy for the Baltimore City Health Department; Dr. Thomas Farley, Philadelphia’s health commissioner; Michael McMahon, district attorney of Richmond County, representing the New York City borough of Staten Island; and Cynthia Reilly, director of Pew’s substance use prevention and treatment initiative.
- Expand the use of naloxone to prevent overdose deaths. Naloxone is a prescription drug that can save lives by reversing the effects of an opioid overdose. It is available to anyone in Pennsylvania, New York, Maryland, and most other states at any pharmacy, without a prescription. But price is an issue: Narcan, the most popular brand of naloxone, costs $150 per dose, although it is covered by most insurance plans with a $40 copay. Behrle pointed out that generic versions of naloxone are far less expensive in other countries.
- Push for fewer opioid prescriptions, while maintaining effective pain management. Physicians and other health care providers legally prescribe opioids to manage patients’ pain. In some instances, such prescriptions can lead to misuse and dependence. While reports indicate that opioids are now being prescribed less often, the panelists agreed that further reductions would be beneficial. Philadelphia, Baltimore, and New York City have sued the pharmaceutical companies that manufacture and distribute opioids, saying the companies overstated the benefits and understated the risks of prescribing the drugs.
- Increase access to medication-assisted treatment. The panelists agreed that medication-assisted treatment is the gold standard for treating opioid use disorder. With this therapy, the patient receives another drug daily—methadone, buprenorphine, or naltrexone—to relieve withdrawal symptoms and/or block the euphoric effects of opioids, including illegal substances such as heroin, and gets counseling simultaneously. Reilly noted that opioid use disorder should be seen in the same way as other chronic diseases, such as diabetes and high cholesterol, for which long-term use of medications is appropriate. The panelists agreed that these medications can help patients struggling with the disorder lead more productive lives at work and in their communities.
- Reduce barriers to treatment. The panelists discussed several barriers to treatment, which they collectively wanted to see reduced. One is cost—to individuals and to state and local governments. Behrle said the ideal solution would be federal legislation similar to the Ryan White Comprehensive AIDS Resources Emergency Act, which covered uninsured and underinsured patients dealing with that disease. Another is the availability of treatment options and public awareness of them. For instance, Farley said that some people seeking treatment in Philadelphia say they cannot find it, even when options are available.
- Use contact with the criminal justice system as an opportunity for intervention. Any contact with the criminal justice system—whether it’s an encounter with a police officer, an arrest, or a trip to jail—represents a chance for someone who is struggling with opioid dependency to get help. Under McMahon’s leadership, Staten Island has instituted a Heroin Overdose Prevention & Education (HOPE) program that diverts individuals arrested for possession into treatment before they are arraigned; if they complete it, the arrest is permanently sealed. A similar program, known as Police-Assisted Diversion, is being tried in one Philadelphia police district.
- Acknowledge that the impact of the problem goes far beyond the overdose death rate. As the discussion highlighted, some people using opioids are not functioning well in the workplace; others become homeless. Babies exposed to opioids in the womb experience painful withdrawal symptoms after birth. Domestic violence occurs, and families fall apart. All of these have impacts on society that will be felt for years.
- Government agencies must work together. The problem is multifaceted, involving a variety of agencies, some of which are not accustomed to working together. In Staten Island, McMahon said he encountered some resistance from the city’s Health Department when he, as a law enforcement official, sought to get involved in what was perceived to be a public health problem. In Philadelphia, as Farley noted, overall responsibility for the opioid crisis rests with the Health Department, while treatment facilities fall under the Department of Behavioral Health and Intellectual Disability Services.
- Safe-injection sites may have benefits but can be difficult for communities to accept. Philadelphia is considering the creation of a site where users would be allowed to inject drugs under supervision, with treatment and counseling close at hand. The proposed facility, which faces legal hurdles, would be the first of its kind in the U.S. Panelists cited evidence from a similar site in Vancouver, Canada, which they said has shown that such a place can save lives and reduce the number of people using drugs on the street. But there is considerable opposition among leaders in communities where a site might be located, and some are skeptical that the positive outcomes in Vancouver would be replicated in Philadelphia.
- Efforts need to be made to reduce the stigma of opioid dependence. Stigma is a problem, Reilly said, because it makes some individuals who have been hiding their opioid dependence and misuse reluctant to seek treatment for fear of repercussions at home or in the workplace. The panelists noted that many people, among the general public and even in the health care system, still see opioid dependence as a personal failing, not a disease.
Watch the full panel discussion below to learn more.


America’s Overdose Crisis
Sign up for our five-email course explaining the overdose crisis in America, the state of treatment access, and ways to improve care
Sign up

‘No Silver Bullet’ for Opioid Crisis in Philadelphia, Other Urban Areas
A mix of education, treatment, and other measures shows promise, experts say










