Can Biosimilar Drugs Lower Medicare Part B Drug Spending?
Leveraging new drug alternatives could reduce costs
Overview
The use of biosimilars—biological products that are highly similar to a biologic drug already approved by the Food and Drug Administration (FDA)—has the potential to reduce drug spending in Medicare Part B,1 which totaled $21.5 billion in 2014.2 However, savings to Medicare will depend on the extent to which biosimilars have lower prices than biologics—which, unlike conventional drugs, are proteins or other materials derived from living cells— and the rate at which providers adopt them. Alternative payment policies, including the use of either a consolidated payment rate or an approach known as the least costly alternative (LCA), could further reduce Part B pharmaceutical costs. Using these policies depends on whether biosimilars can be safely and effectively substituted for biologics.
The current payment approach
Medicare payment to providers for Part B drugs is based on a drug’s average sales price (ASP) for all purchasers.3 Payment for most Part B drugs is set at ASP plus an add-on of 4.3 percent.4 By statute, however, providers who administer biosimilars are reimbursed at the ASP plus 4.3 percent of the ASP of the reference biologic—the drug on which the biosimilar is based.5 By paying the same add-on rate for biologics and their biosimilars, the Centers for Medicare & Medicaid Services (CMS) creates equal financial incentives for providers who are choosing between a reference biologic and a biosimilar.
Alternative approaches
A consolidated payment rate
The Medicare Part B program, in contrast to its payment policy for biologics, reimburses providers the same amount for brand and generic versions of conventional drugs. This consolidated rate is based on the volume- weighted ASP of all brand and generic versions of a medicine.6 If a similar approach were adopted for reference biologics and biosimilars, Part B drug spending could be reduced if providers responded by increasing their use of biosimilars over reference biologics (or increasing the use of the reference product if it were available at lower cost). However, the adoption of a consolidated payment rate would have no effect on costs if providers did not increase uptake of the lower-cost product. Notably, Medicare savings from a consolidated payment rate would be greatest compared to the current payment policy when biosimilar use, or uptake, was low, and would be smallest when biosimilar use was high.
A consolidated payment approach, which would effectively decrease Medicare payment for higher-cost reference biologics and increase payment for lower-cost biosimilars, would create a financial incentive for providers to switch to the latter. According to the office of the inspector general, Medicare’s use of a consolidated payment rate has reduced the price it pays for branded conventional drugs by nearly 60 percent in two years.7
The least costly alternative approach
Research shows that an LCA approach—in which the payment rate for a higher-cost therapy is set at the payment level of a lower-cost, therapeutically comparable alternative—could also reduce Medicare Part B costs on reference biologics and their biosimilars.8
This policy has the potential to reduce drug spending by a greater amount than the consolidated payment approach, which takes into account the ASP of a more expensive reference biologic. And LCA does not, unlike the consolidated payment approach, rely on increased uptake of biosimilars to generate cost savings. Assuming no change in overall utilization, total Medicare spending on therapeutically comparable drugs in an LCA grouping, including reference biologics and their biosimilars, would be the same regardless of biosimilar uptake.
Additional considerations with alternative approaches
Both the consolidated approach and LCA would be practical not only for products that FDA determined were interchangeable, but also potentially for biosimilars that were not approved as interchangeable by FDA.9 Because research shows that some biosimilars have the same efficacy and safety as FDA-approved reference biologics,10 some commercial insurers in the United States have implemented policies to favor coverage of biosimilars over reference biologics—even though FDA has not determined that they are interchangeable.11
Nevertheless, the consolidated approach and LCA may not always be appropriate if a biologic and its biosimilars cannot be substituted, such as when there are safety concerns with switching patients to a biosimilar. It is also possible that the interchangeability of a reference biologic and biosimilar will differ depending on the indication for which the drug is prescribed.
Reductions in Medicare Part B payment may also increase the number of providers who are “underwater” when they administer a reference biologic, because the payment they receive from Medicare is less than their cost of acquiring the drug from a wholesaler or directly from the drug company. This could lead to providers choosing to stop treating their patients with biologics for which there are no lower-cost, interchangeable biosimilars, thus limiting patient access to drug therapies.
Furthermore, developers of reference biologics are likely to explore ways to maintain their market share as new biosimilars are developed. One approach might be to alter or improve a biologic—such as by making changes to reduce the number of doses—in order to extend patent protections or exclusivity that could prevent biosimilar competition. For example, although the main patents for Enbrel (etanercept), a drug used to treat rheumatoid arthritis, have expired, new patents granted in 2011 will potentially delay biosimilar competition through 2029.12
The manufacturers of reference biologics could also respond to competition from biosimilars, as well as to new payment policies, by lowering the price of their products—as the manufacturer of Aranesp, a drug to treat chronic kidney disease and cancer, has done in markets outside the United States.13
Policy options for biosimilars in Medicare Part B
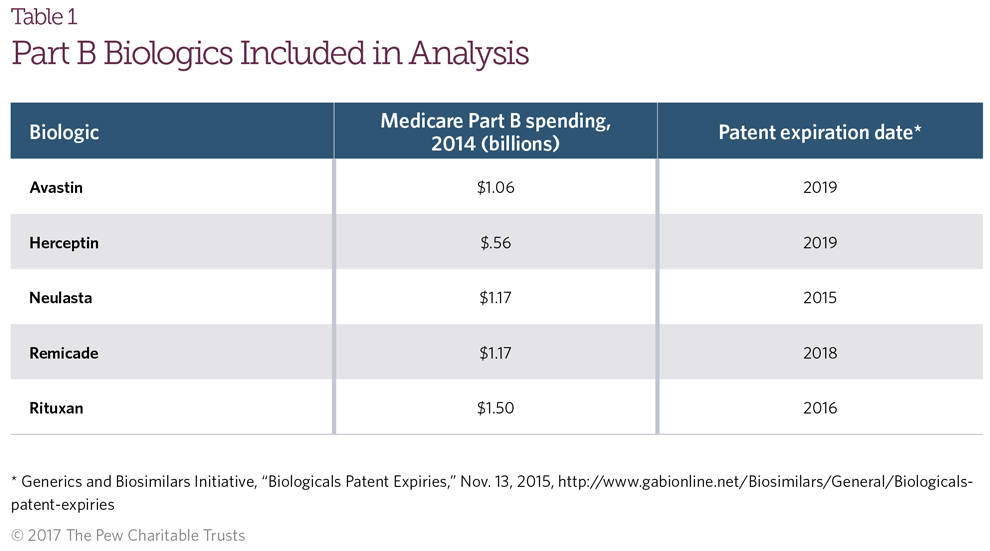
The following data examining the potential one-year effect of the current policy, as well as the potential one- year impacts of the consolidated payment and LCA policies on Part B drug costs, focus on five biologics covered under Medicare Part B: Avastin (bevacizumab), Herceptin (trastuzumab), Neulasta (pegfilgrastim), Remicade (infliximab), and Rituxan (rituximab).14 These reference biologics were selected based on their costs to Medicare Part B,15 an assessment of the number of biosimilars currently in development for each,16 and anticipated patent expirations (Table 1).
In 2014, annual Part B spending on these five biologics totaled $5.47 billion, which is based on the payment rate of ASP plus 4.3 percent. The Pew Charitable Trusts estimates that the ASP of each drug, when combined, accounts for approximately $5.25 billion of this total amount, while $226 million can be attributed to the 4.3 percent add-on payment.
In constructing a model to estimate drug spending, the following assumptions were made about pricing, utilization, and the Part B biologic market:
- Baseline spending on the five reference biologics is based on 2014 Medicare Part B data obtained from the CMS’ Medicare Drug Spending Dashboard.
- The total utilization of biologics (reference biologics and biosimilars) remains constant at 2014 rates.
- The biologics are assumed to have lost exclusivity and patent protection, and to have begun facing competition from biosimilars. Biosimilars are approved for the same indications as those for which their respective reference biologics are approved, and not for any additional indications.
- The price of each reference biologic remains constant at the average of its 2014 payment rate. Reference biologic and biosimilar ASPs do not change during the year.
- Biosimilar prices are 35 percent lower than those of reference biologics. This pricing differential is consistent with estimates reported in other studies and uptake rates for some biosimilars in Europe.17
- Under the current payment policy, use of biosimilars is 50 percent of the total biologic utilization. This assumption is based on the uptake rate of some biosimilars in Europe and market penetration assumptions used in other analyses.18
- Patients taking medications not included in this analysis will not switch to any of the included biologics or biosimilars.
- There is no shift in the coverage of drugs from Medicare Part B to Part D.
- Biosimilar prices and uptake are not affected by the number of biosimilars available. The launch of multiple biosimilars for the same reference biologic does not create any additional effect on prices or utilization.
- Under LCA, the payment amount for a reference biologic and its biosimilars is based on the ASP of biosimilars plus an add-on of 4.3 percent.
- Compared with the current payment policy, the consolidated approach increases biosimilar use by 10 percentage points (from 50 to 60 percent). Though evidence is limited, this assumption is informed by available research on changes in utilization in response to new Medicare Part B payment rates for pharmaceuticals.19
- Under the consolidated payment policy, the payment rate for a reference biologic and its biosimilars is based on the volume-weighted average ASP plus an add-on payment equal to 4.3 percent of this volume- weighted amount.
- Patients pay for 20 percent of the cost of treatment with biologics. In estimating potential costs to patients, reductions in out-of-pocket costs for patients with supplemental Medigap insurance coverage were excluded.
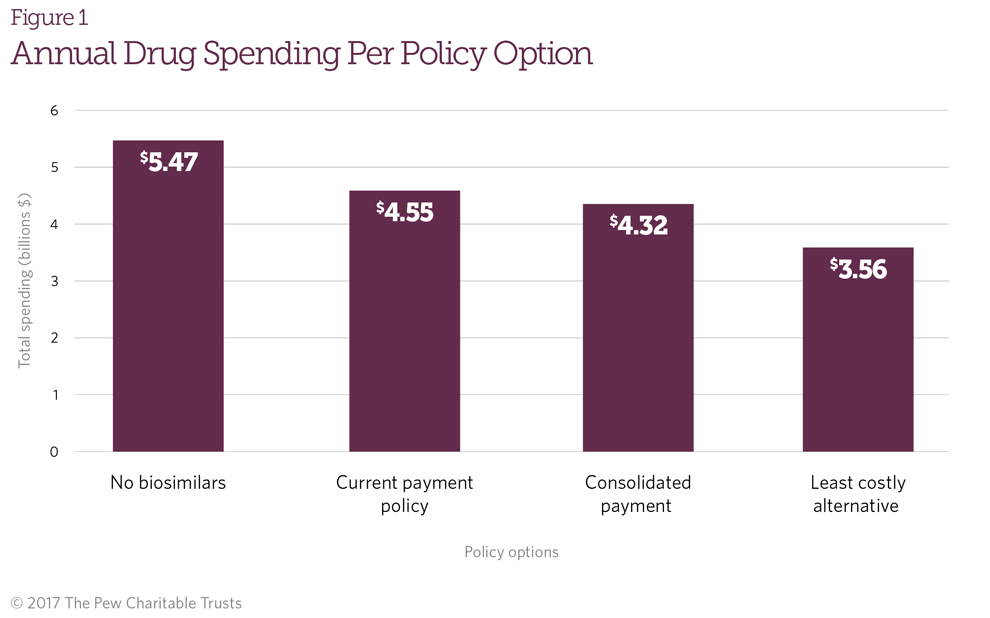
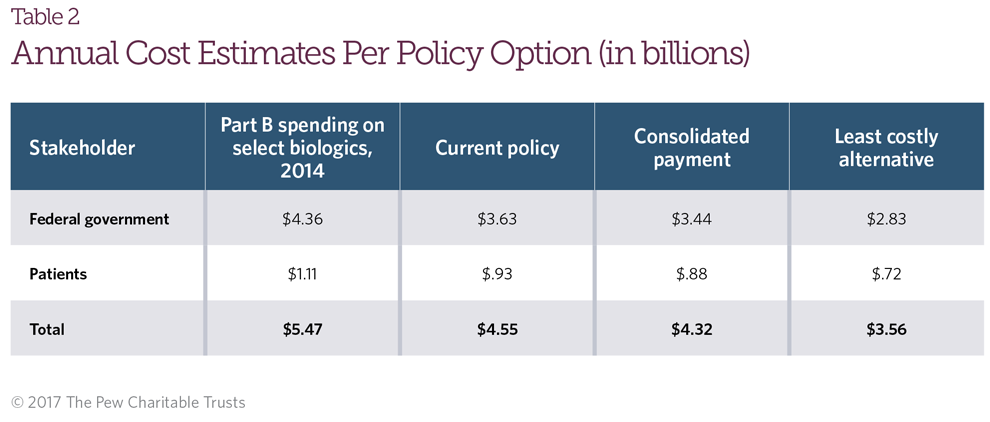
Under these base case assumptions, the availability of biosimilars under Medicare’s current payment policy would reduce annual spending for these five drugs from $5.47 billion to $4.55 billion, or approximately 17 percent (Figure 1). The consolidated payment approach would reduce annual spending to $4.32 billion, for a savings of 21 percent, while an LCA policy would reduce annual spending to $3.56 billion, for a savings of 35 percent. Costs to the federal government and Medicare patients under the various payment models are displayed in Table 2.
These estimates are sensitive to assumptions on biosimilar pricing, biosimilar uptake, and provider responsiveness to payment rate changes under a consolidated payment approach. Sensitivity analyses were conducted to evaluate the impact of each of these assumptions while keeping all other assumptions constant.
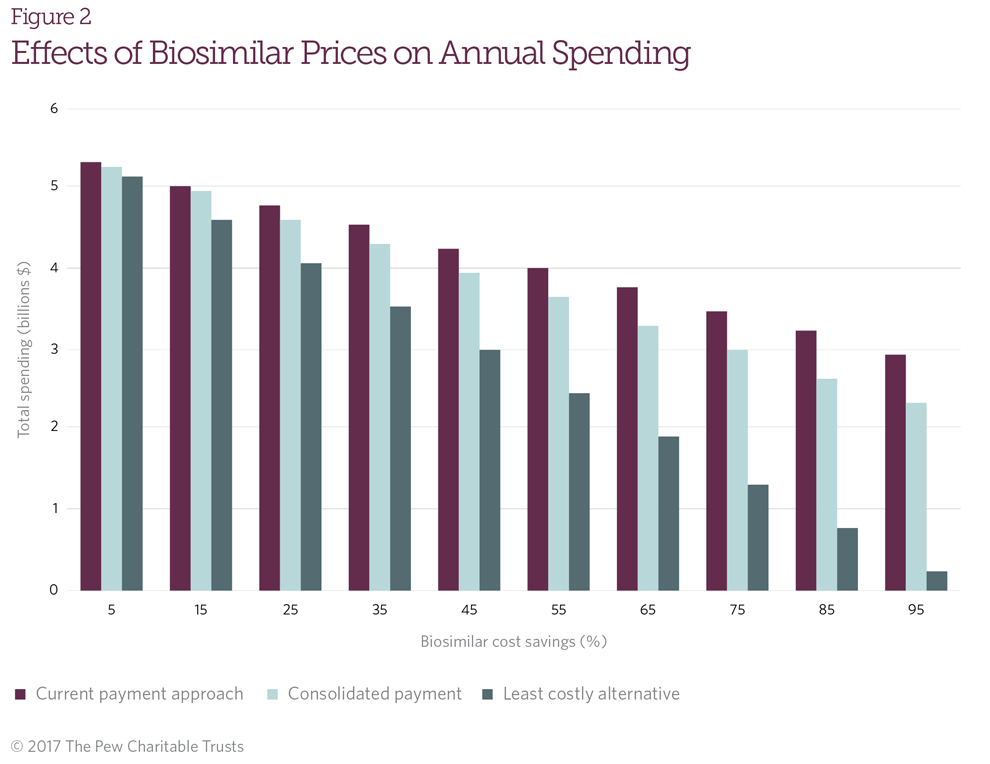
- Biosimilar pricing: When biosimilar prices are close to that of a reference biologic, cost savings are reduced and drug spending is higher (Figure 2). This trend was detected for all three policies.
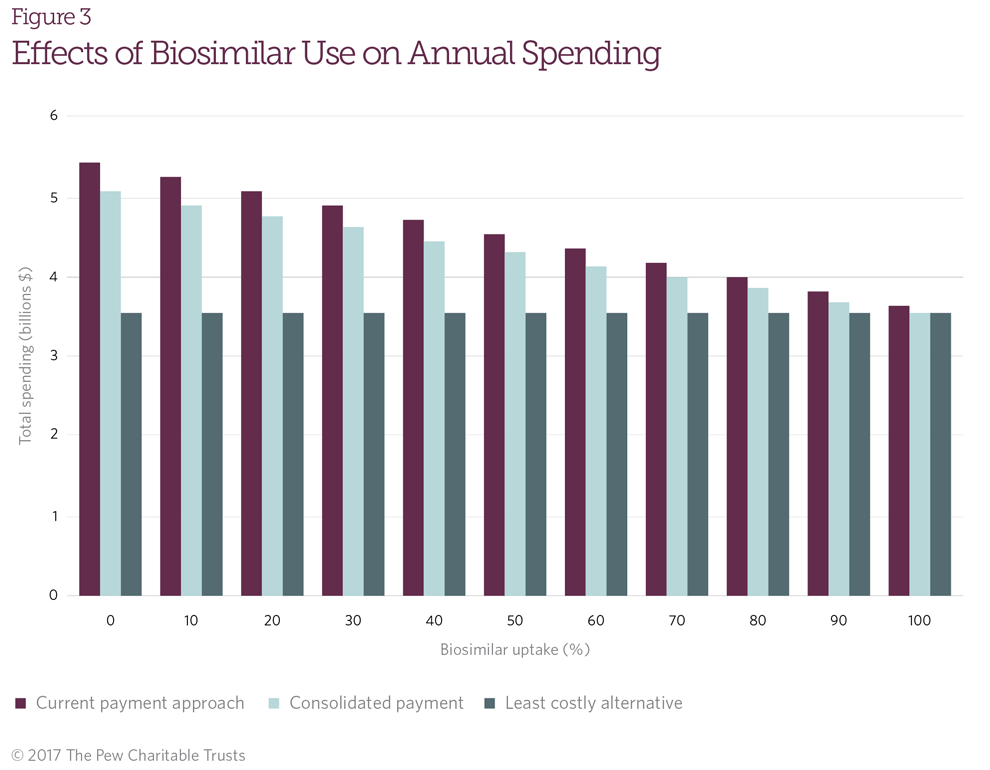
- Biosimilar use: The magnitude of savings generated both with the current payment policy and with the consolidated payment approach is sensitive to assumptions on biosimilar uptake (Figure 3); increased biosimilar uptake would result in lower spending on drugs under both payment strategies. However, annual spending under LCA would total $3.56 billion regardless of biosimilar uptake.
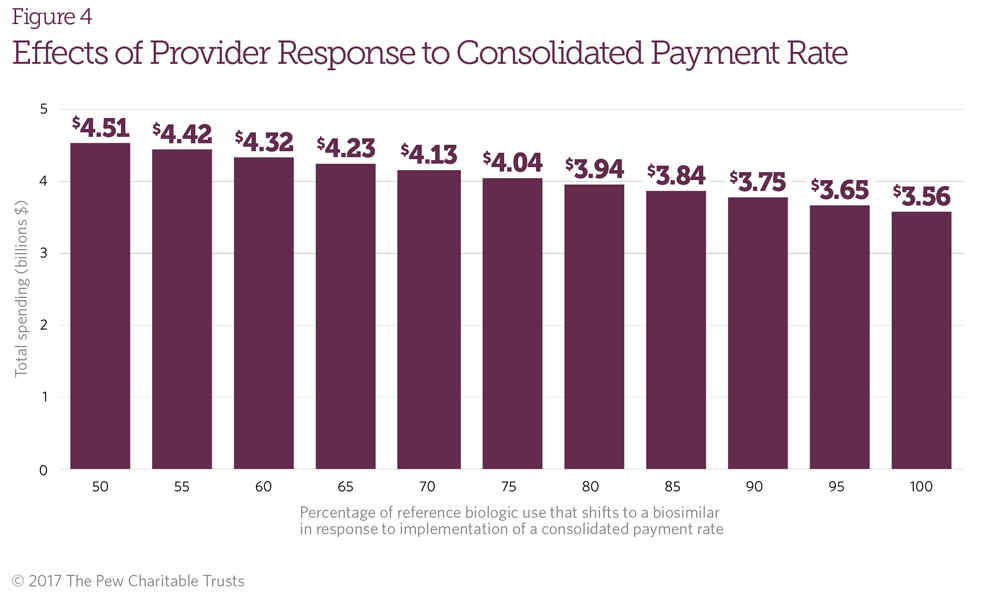
- Provider response to a consolidated payment approach: The analysis also demonstrates that if providers were more responsive to a reduction in payment for reference biologics resulting from the consolidated payment approach, then cost savings would be greater (Figure 4). For example, if all providers responded by switching to the biosimilar, the cost savings under a consolidated payment approach would be equal to savings generated under LCA.
Ensuring appropriate patient access to reference biologics
The policy alternatives discussed in this brief would reduce Medicare payment for biologics when there are lower-cost biosimilars available. However, some stakeholders have expressed concern that reducing Medicare payment could inappropriately limit patient access and lead to worse health outcomes.20 For this reason, it is important that the decision to implement either LCA or consolidated payment be informed by clinical evidence.
For example, patients already being treated with a reference biologic should not be switched to a biosimilar unless there is evidence demonstrating the interchangeability of the two products. If the products are not interchangeable, paying providers based on the consolidated payment approach or LCA could inappropriately limit patient access to necessary care.
However, there are other circumstances, such as newly diagnosed patients, in which treatment with a biosimilar is appropriate. In these cases, policymakers should consider using new approaches to manage health care costs. Tools such as consolidated payment and LCA have the potential to increase competition and lower Medicare drug spending on biologics and biosimilars that produce similar clinical outcomes.
Conclusion
Under Medicare’s current payment policy, providers generally have equal financial incentives to administer either reference biologics or biosimilars to patients. Alternative policies, such as those described here, have the potential to generate greater savings to Medicare. However, policymakers should consider clinical evidence, including research on interchangeability of biologics and biosimilars, before developing and implementing new policies.
Endnotes
- Medicare Part B covers physician-administered drugs that are typically given in a physician’s office, clinic, or hospital outpatient department.
- Centers for Medicare & Medicaid Services, “Medicare Drug Spending Dashboard,” Dec. 21, 2015, https://www.cms.gov/Newsroom/MediaReleaseDatabase/Fact-sheets/2015-Fact-sheets-items/2015-12-21.html.
- 42 U.S.C. § 1395W-3A, “Use of Average Sales Price Payment Methodology,” https://www.law.cornell.edu/uscode/text/42/1395w-3a?qt- us_code_temp_noupdates=0#qt-us_code_temp_noupdates. Average sales price (ASP) is defined as a manufacturer’s sales of a drug to all purchasers in the United States in a calendar quarter divided by the total number of units of the drug sold by the manufacturer in the same quarter.
- Medicare Payment Advisory Commission, Report to Congress: Medicare and the Health Care Delivery System (June 2015), http:// www.medpac.gov/docs/default-source/reports/june-2015-report-to-the-congress-medicare-and-the-health-care-delivery-system.pdf?sfvrsn=0. By statute, payment for Part B drugs is set at ASP plus 6 percent. However, the sequester reduces the payment rate to ASP plus 4.3 percent. According to the commission, there is no consensus on the original intent of the 6 percent add-on payment.
- For example, if a reference biologic has an ASP of $200 and a biosimilar has an ASP of $100, the Medicare Part B payment for the two products would be $208.60 and $108.60, respectively. The add-on payment for both products is determined based on the 4.3 percent of the reference biologic ASP, which equals $8.60.
- A volume-weighted ASP takes into account the total volume and price of each drug. For example, if Brand A with an ASP of $20 has 80 percent of the market and Generic B with an ASP of $10 has 20 percent of the market, then the volume-weighted ASP for these two products would be $18 ([$20 x 0.8] + [$10 x 0.2] = $18).
- Office of Inspector General, Department of Health and Human Services, Medicare Payments for Newly Available Generic Drugs (2011), http://oig.hhs.gov/oei/reports/oei-03-09-00510.pdf.
- The Pew Charitable Trusts, “The ‘Least Costly Alternative’ Approach for Payment of Medicare Part B Drugs: How Different Reimbursement Models Could Affect Drug Prices” (March 2016), http://www.pewtrusts.org/en/research-and-analysis/fact-sheets/2016/03/the-least-costly-alternative-approach-for-payment-of-medicare-part-b-drugs.
- 42 U.S.C. § 262(k)(4), “Regulation of Biological Products,” https://www.law.cornell.edu/uscode/text/42/262. FDA can determine that a biosimilar is interchangeable with a reference biologic if the two products produce the same health outcomes in any given patient and if there is no safety risk or diminished efficacy in switching between the reference biologic and the biosimilar.
- Francine Chingcuanco et al., “Bioequivalence of Biosimilar Tumor Necrosis Factor- Inhibitors Compared With Their Reference Biologics: A Systematic Review,” Annals of Internal Medicine 165, no. 8 (2016): 565–74, http://dx.doi.org/10.7326/M16-0428.
- Joseph Walker and Paul Ziobro, “CVS Drops Coverage of 2 Branded Biotech Drugs in Favor of Copies,” The Wall Street Journal, Aug. 2, 2016, http://www.wsj.com/articles/cvs-drops-coverage-of-2-branded-biotech-drugs-in-favor-of-copies-1470176277.
- Emily Wasserman, “Amgen Targets Sandoz’s Enbrel Biosim With Patent Infringement Suit,” FiercePharma, March 2, 2016, http://www.fiercepharma.com/legal/amgen-targets-sandoz-s-enbrel-biosim-patent-infringement-suit.
- Thomas Gryta, “Hospira Learning Valuable Lessons in European Biosimilar Market,” Dow Jones Newswires, Oct. 1, 2009, http://www.advfn.com/nasdaq/StockNews.asp?stocknews=TEVA&article=39719143.
- Avastin and Herceptin are approved to treat cancer; Neulasta is approved to prevent infection in chemotherapy patients; Remicade is approved to treat rheumatoid arthritis and other autoimmune disorders; and Rituxan is approved to treat cancer and rheumatoid arthritis.
- The five biologics accounted for 25 percent of Medicare Part B drug spending in 2014.
- IMS Institute for Healthcare Informatics, Medicines Use and Spending in the US: A Review of 2015 and Outlook to 2020 (April 2016), http://www.imshealth.com/en/thought-leadership/quintilesims-institute/reports/medicines-use-and-spending-in-the-us-a-review-of-2015-and-outlook-to-2020#form. These five biologics are among those with the greatest number of biosimilars in development.
- IMS Institute for Healthcare Informatics, Delivering on the Potential of Biosimilar Medicines: The Role of Functioning Competitive Markets (March 2016), http://www.imshealth.com/files/web/IMSH Institute/Healthcare Briefs/Documents/IMS_Institute_Biosimilar_Brief_March_2016.pdf; and Andrew W. Mulcahy, Zachary Predmore, and Soeren Mattke, “The Cost Savings Potential of Biosimilar Drugs in the United States,” Rand Corp. (2014), https://www.rand.org/content/dam/rand/pubs/perspectives/PE100/PE127/ RAND_PE127.pdf.
- Ibid.
- Mireille Jacobson et al., “How Medicare’s Payment Cuts for Cancer Chemotherapy Drugs Changed Patterns of Treatment,” Health Affairs 29, no. 7 (2010): 1391–9, http://content.healthaffairs.org/content/29/7/1391.full. Though evidence is limited, research by Jacobson and colleagues suggests that providers do respond to changes in financial incentives. In response to Part B drug payment cuts, providers switched from dispensing drugs with the largest cuts in profitability to other drugs with smaller cuts. In the current analysis of the consolidated approach, it is assumed that providers will switch from dispensing a reference biologic to a biosimilar due to the increase in payment for the latter and reduction in payment for the former.
- Kerry Young, “MedPAC Stirs Talk of Cost-Based Approach of Some Drugs,” Washington Health Policy Week in Review, Sept. 15, 2014, http://www.commonwealthfund.org/publications/newsletters/washington-health-policy-in-review/2014/sep/sep-15-2014/medpac-stirs-talk-of-cost-based-approach-on-some-drugs.


America’s Overdose Crisis
Sign up for our five-email course explaining the overdose crisis in America, the state of treatment access, and ways to improve care
Sign up
Policies to Accelerate Approvals of Generic and Biosimilar Drugs
Strategies aim to bolster competition by improving generic manufacturers’ access to brand name products