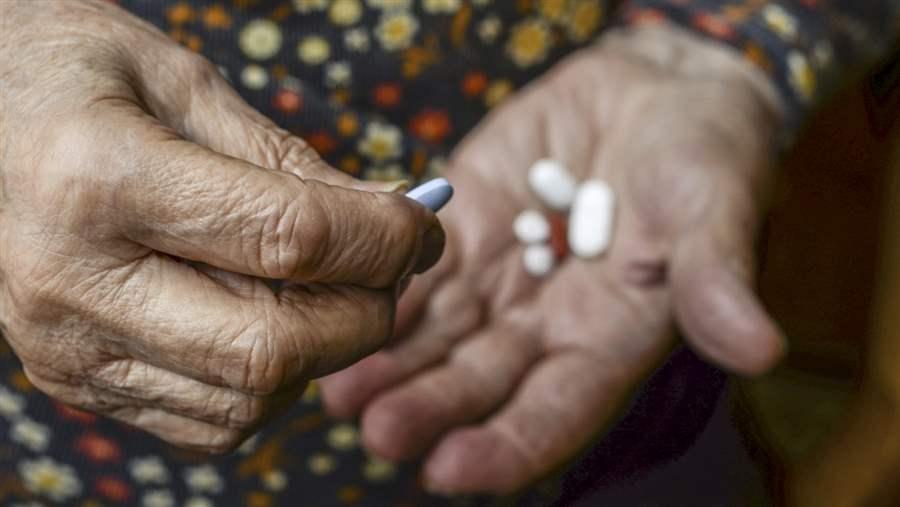
Medicare Must Do More to Protect Beneficiaries Susceptible to Opioid-Related Harms
The agency’s recent proposal would do little to curb the opioid crisis in this population
In November, the Centers for Medicare & Medicaid Services (CMS) issued a proposed rule intended to protect Medicare beneficiaries who are at risk from opioid misuse. The rule sets expectations for insurers developing drug management programs known as patient review and restriction (PRR) programs, which are used to identify at-risk patients and assign them to designated prescribers and/or pharmacies for their controlled substance needs. While welcome, this rule as proposed fails to adequately protect these patients, and must be improved.
PRRs are widely used in Medicaid and commercial insurance because they can improve care coordination, reduce opioid prescriptions and visits to multiple doctors and emergency rooms, and bring down health care costs.
These programs would also be valuable in Medicare. The U.S. Department of Health & Human Services’ Office of Inspector General found that almost 90,000 beneficiaries were at serious risk of opioid misuse or overdose in 2016, either because they were receiving high doses of opioids for extended periods of time, or were visiting multiple prescribers and pharmacies to obtain these medications.
Unfortunately, the proposed rule has significant shortcomings, as Pew noted in a recent letter. Specifically:
- The draft regulations describe prescriber-based PRR programs as a “tool of last resort,” and prohibit their use until at least six months after the CMS identifies potentially harmful opioid use. This contradicts what the Comprehensive Addiction and Recovery Act (CARA)—the legislation that allows for the use of these programs—sought to do, by giving insurers a proactive tool to work with prescribers to curb harmful use of opioids in the Medicare population.
- The proposed rule also recommends that patients not be enrolled in PRR programs unless they obtain high-dose opioid prescriptions from at least four prescribers and at least four pharmacies in a six-month period. These thresholds are higher than Medicare’s current parameters for identifying risky behavior, meaning that insurers may not identify all beneficiaries at risk for opioid-related harm.
- In addition, the rule does not allow insurers to consider prescriptions for other classes of drugs, such as benzodiazepine sedatives that, when used in combination with opioids, are associated with an increased risk of overdose-related death.
- Finally, the regulations require that beneficiaries be automatically discharged from PRR programs, rather than having insurers assess patient risk before determining if enrollment is no longer necessary.
The proposed rule also has strengths, including strong patient protections. For example, it requires that beneficiaries enrolled in PRR programs have reasonable access to their prescribed medications, which means that patients can provide input on selected prescribers and pharmacies. Furthermore, enrollees with special circumstances—such as those who have multiple residences—can select providers in each location. And individuals who wish to appeal their enrollment in the PRR program can use Medicare’s existing appeals process.
CARA provided the CMS with new tools to protect Medicare beneficiaries from opioid-related harms. Unfortunately, without major changes, the proposed regulations would not fully achieve this goal.
Cynthia Reilly directs Pew’s substance use prevention and treatment initiative.


America’s Overdose Crisis
Sign up for our five-email course explaining the overdose crisis in America, the state of treatment access, and ways to improve care
Sign up
Pew Comments on Proposed Regulations for Medicare Part D Drug Management Programs
Proposal would do little to curb opioid misuse in the Medicare population
Patient Review and Restriction Programs in Medicaid
Expert panel recommendations to help curb misuse of prescription drugs