Advancing Integrity in Medical Education
A new national initiative to improve conflict-of-interest policies at academic medical centers
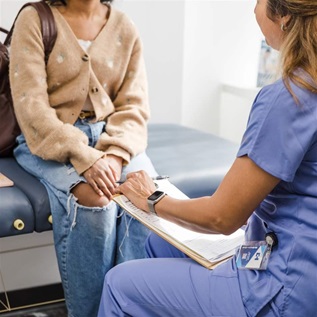
The challenge
In 2012, the drug industry spent more than $27 billion marketing medicines directly to doctors.1 Gifts and payments from industry to doctors can affect the choices they make when they treat patients, and the usual result is the prescription of new, high-priced, brand-name medications rather than well-established generic drugs that have longer track records of safety.2,3,4
A solution based in education
The Pew Charitable Trusts is working to decrease the influence of pharmaceutical marketing on doctors' practices. With a three-year grant from the Attorney General Consumer and Prescriber Education Grant Program, Pew is collaborating with the American Medical Student Association, Community Catalyst, and the National Physicians Alliance to improve conflict-of-interest policies within the 161 medical schools and 400 major teaching hospitals in the United States. Together, we are developing a set of best-practice standards, determining whether academic medical centers have adopted these practices, and providing technical assistance to these institutions. Our goal is that 75 percent of academic medical centers will implement strong conflict-of-interest policies by 2014.
The following resources and opportunities are available:
-
American Medical Student Association's Scorecard 2014: A tool for evaluating institutions' conflict-of-interest policies annually. (The 2014 version was revised and expanded to include teaching hospitals).
-
Expert task force on medical conflicts of interest: A team of leaders in the medical institutions that will create policy recommendations for medical schools and teaching hospitals, which will appear in various publications.
-
National grand rounds: Events with expert speakers who share their experiences on conflict-of-interest topics.
(Lectures are Web-archived, and free continuing medical education credits are available.)
-
Leadership development calls: Professional conference calls to learn about conflict-of-interest topics such as the Physician Payments Sunshine Act, pharmaceutical marketing techniques, and ways to strengthen policies at academic medical centers. (Web archive available.)
-
Tool kits: Customizable materials that can help institutions improve their conflict-of-interest policies.
-
Micro-grants: Funding opportunities for medical students to implement conflict-of-interest projects on their campuses.
Who we are
Pew's prescription project is the lead organization coordinating the activities of the Partnership to Advance Conflict-Free Medical Education. The prescription project seeks to ensure transparency in physician-industry relationships and promotes policies to reduce or manage conflicts of interest that could affect patient care. Contact Sallyann Bergh at 202-540-6783 or [email protected].
The American Medical Student Association is a student-governed national organization committed to representing the concerns of physicians-in-training. Since 2007, the association's annual scorecard has tracked conflict-of-interest policies in medical schools, using a letter grade to evaluate their adequacy. The scorecard has been an effective tool for encouraging schools to adopt model policies.
Community Catalyst is a national nonprofit advocacy organization whose first priority is high-quality, affordable health care for all. It has worked closely with Pew and the American Medical Student Association on improving conflict-of-interest policies in medical settings nationwide.
The National Physicians Alliance is a nonprofit membership and advocacy organization that represents physicians across medical specialties who share a commitment to professional integrity and health justice. Its “Unbranded Doctor” campaign provides guidance and tools for health-care practitioners who value practicing medicine free from undue influence from the pharmaceutical industry.
This partnership and related materials were made possible by a grant from the state Attorney General Consumer and Prescriber Education Grant Program, which is funded by the multistate settlement of consumer fraud claims regarding the marketing of the prescription drug Neurontin.
References
1 Cegedim Strategic Data, “2012 U.S. Pharmaceutical Company Promotion Spending,” accessed April 18, 2013, skainfo.com/health_care_market_reports/2012_promotional_spending.pdf.
2 Erik G. Campbell, Geneveive Pham-Kanter, Christine Vogeli, and Lisa I. Iezzoni, “Physician Acquiescence to Patient Demands for Brand-Name Drugs: Results of a National Survey of Physicians,” JAMA Internal Medicine 173 (2013): 237-239.
3 Marissa King, Connor Essick, Peter Bearman, and Joseph S. Ross, “Medical School Gift Restriction Policies and Physician Prescribing of Newly Marketed Psychotropic Medications: Difference-in-Differences Analysis,” British Medical Journal 346 (2013): 264.
4 Geoffery K. Spurling, Peter R. Mansfield, Brett D. Montgomery, et al., “Information From Pharmaceutical Companies and the Quality, Quantity, and Cost of Physicians' Prescribing: A Systematic Review,” PLoS Medicine 7 (2010): e1000352.
Spotlight on Mental Health
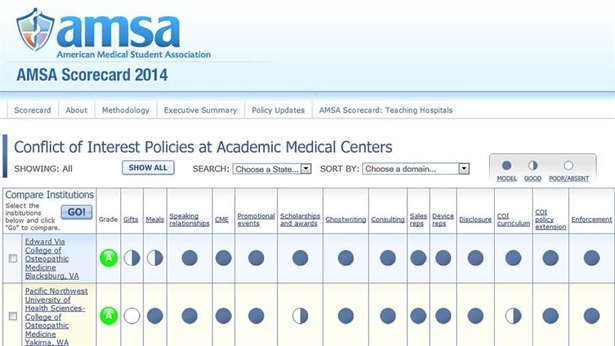
Conflict of Interest Policies at Academic Medical Centers and Teaching Hospitals
AMSA Scorecard 2014MORE FROM PEW
Explore Pew’s new and improved
Fiscal 50 interactive
Your state's stats are more accessible than ever with our new and improved Fiscal 50 interactive:
- Maps, trends, and customizable charts
- 50-state rankings
- Analysis of what it all means
- Shareable graphics and downloadable data
- Proven fiscal policy strategies
Welcome to the new Fiscal 50
Key changes include:
- State pages that help you keep track of trends in your home state and provide national and regional context.
- Interactive indicator pages with highly customizable and shareable data visualizations.
- A Budget Threads feature that offers Pew’s read on the latest state fiscal news.