Health Impact Assessment Can Inform Planning to Promote Public Health
Process offers opportunities for collaboration among planners and public health professionals
 © The Pew Charitable Trusts
© The Pew Charitable TrustsPlanners are at the forefront of efforts to address many of the nation’s most pressing health challenges.
Overview
Land-use and community planning decisions can affect public health.1 This brief introduces planning directors and staff as well as policymakers to health impact assessment (HIA), a process that brings public health considerations into decision-making. It describes how HIAs can add value across a range of topics and summarizes the findings from a review of 134 planning-related HIAs conducted in the U.S. between 2004 and 2014. The Planning and Community Health Center of the American Planning Association (APA) led the review in consultation with the Health Impact Project, a collaboration of the Robert Wood Johnson Foundation and The Pew Charitable Trusts.2
Planning affects health
The places where people live, work, and play influence many of the nation’s most pressing public health determinants—such as levels of income and education and exposure to violence—as well as health outcomes, including respiratory illness, cardiovascular disease, injury, and mental health.3 Planning professionals are in a unique position to promote public health through their work. For example, a jurisdiction’s land-development patterns and zoning policies can directly affect important health determinants, such as the availability and affordability of housing; the presence of pedestrian-friendly neighborhoods; the range of transportation options; levels of crime in a community; and access to education, employment, and other essential goods and services.4
Planners can help jurisdictions anticipate, design, and implement spaces where people live, work, and play in a manner that reduces air pollution, encourages physical activity, provides access to essential services, and preserves green space, all of which are important to health. Additionally, planners can help ensure that health is a priority in decision-making across a range of sectors, because they often work in multidisciplinary teams with other specialists, such as engineers; architects; landscape architects; real estate developers; and transportation, law enforcement, housing, and economic development professionals.
What is health impact assessment?
HIA brings together scientific data, health expertise, and stakeholder input to identify the potential and often-overlooked positive and negative effects on public health of proposed laws, regulations, projects, policies, and programs.5 HIAs provide pragmatic, evidence-based recommendations about how to reduce risks, promote benefits, and monitor the health effects of the implemented decision.6 These assessments have been used to inform decision-making in a range of sectors, including planning, agriculture, criminal justice, economic policy, transportation, and housing.
Planning HIA basics
Who: HIAs involve a range of stakeholders, such as decision-makers, elected and appointed officials, planners, public health practitioners, business owners, residents, and community members, as active participants in the process. Planners can play various roles in assessments depending on their interest and capacity, including being an audience for the information and recommendations, participating on advisory committees, collaborating with health professionals or other partners on the assessment, or initiating and leading HIAs themselves.
What: HIAs take into account environmental, social, and economic factors related to health and evaluate the potential impacts of a proposed project, plan, program, or policy on the health of the community. The HIA process occurs in six steps—screening, scoping, assessment, recommendations, reporting, and evaluation and monitoring—with stakeholder engagement at each phase.
When: HIAs are a method of proactively informing a decision under consideration and can be used to influence any stage of the planning process, including visioning, goal-setting, and the creation and implementation of plans, policies, and projects, as long as the assessment is completed in advance of the decision it seeks to inform.
Where: Planning HIAs can assess health impacts of projects, plans, and policies at the building, street, neighborhood, local, or regional scale.
Why: HIAs can help planning efforts protect and promote the health and well-being of the community and help ensure that health benefits and risks from decisions are equitably distributed. Planners create and strengthen vibrant, sustainable places, and HIAs can support that work by bringing to light potential unintended consequences and opportunities to promote health, and making recommendations to address risks and enhance benefits. HIAs’ emphasis on community engagement can also complement the planning process and create buy-in for adoption and implementation.
How: HIAs employ a variety of data sources, such as demographic and health information and input from stakeholders, to identify the potential health effects of planning decisions, with special attention paid to certain target populations such as seniors, children, and low-income communities. HIAs can be fairly quick, using a “rapid” or “desktop” model over a few weeks or months, or they can use a longer, more comprehensive approach, taking several months to more than a year to complete.7
HIA in planning
Approximately one-third (134) of all HIAs completed in the U.S. between 2004 and 2014 looked at planning decisions to better understand their impacts on the health of neighborhoods and communities.8 Of these HIAs:
- 63 percent focused on a specific plan, such as a comprehensive or forest-management plan.
- 24 percent looked at a planning-related policy.
- 13 percent considered a project or an action undertaken to implement a plan or policy.
These HIAs assessed a diverse set of planning topics, reflecting the varied and comprehensive nature of the planning field, including:
- Land use.
- Development regulations.
- Public finance.
- Disaster mitigation.
- Climate change.
The review excluded planning HIAs focused solely on housing or transportation because they have been summarized in previous studies.9 It did, however, include HIAs that addressed housing or transportation as a component of broader planning efforts.
Table 1 provides a summary of selected planning HIAs from the APA review to capture the breadth and scope of the decisions HIAs can inform and the health effects they can address.
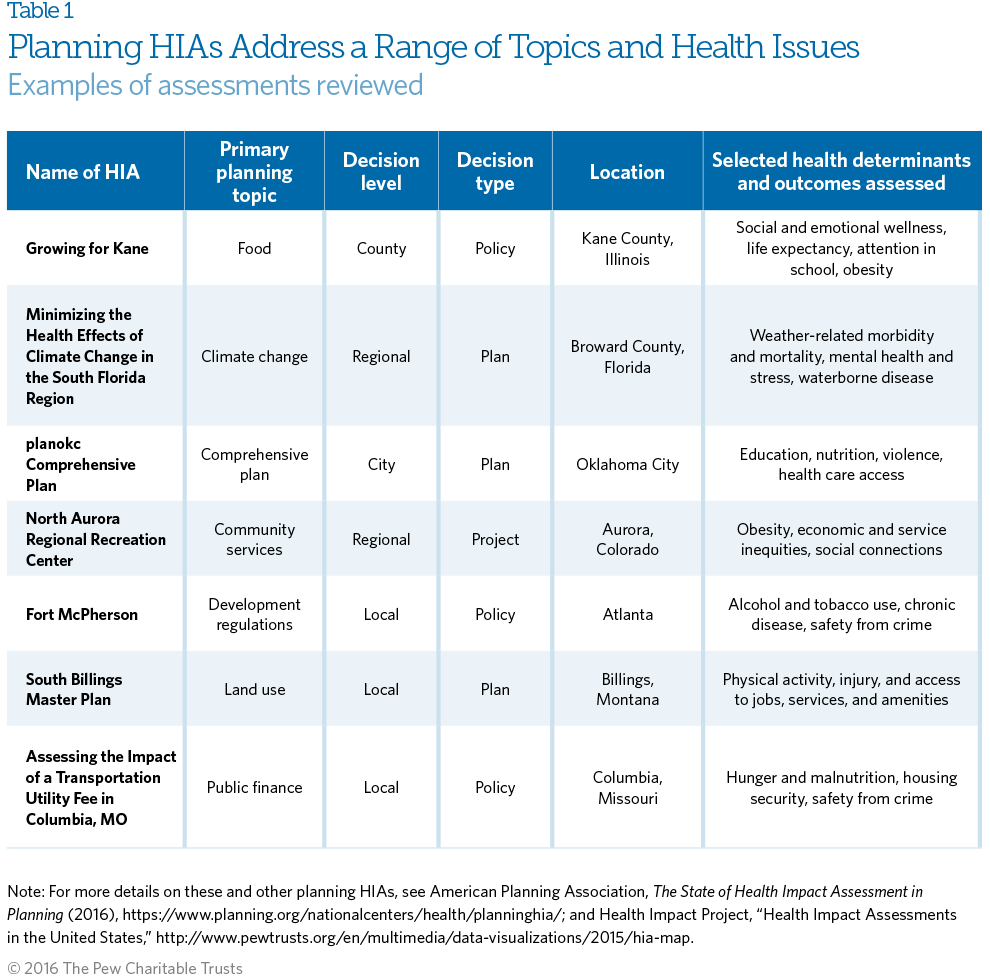
Approximately one-third (134) of all HIAs completed in the U.S. between 2004 and 2014 looked at planning decisions to better understand their impacts on the health of neighborhoods and communities.
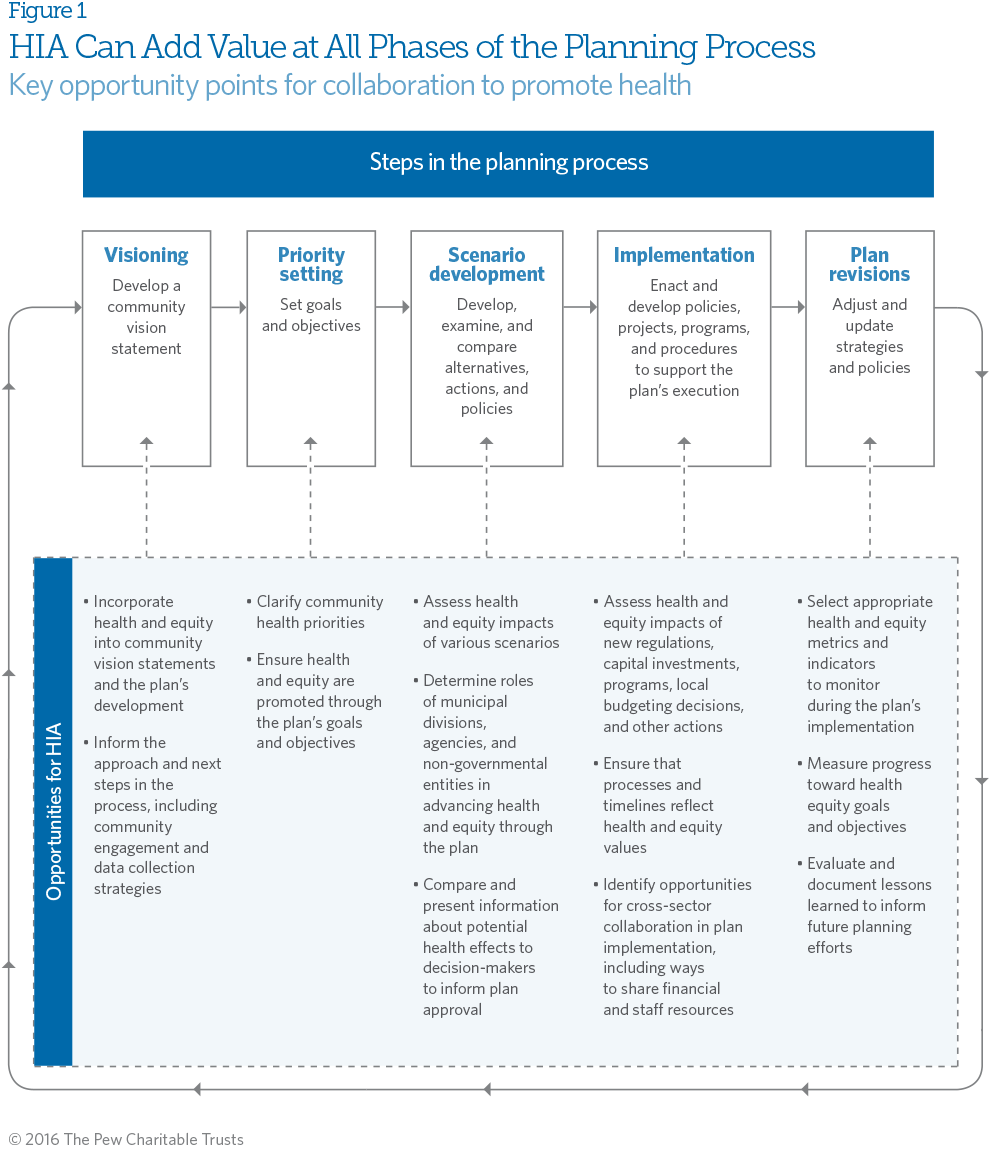
HIAs can add value to the planning process in four key ways: improving data, promoting citizen involvement, providing opportunities for cross-sector collaboration, and reframing contentious issues around shared health goals. (See Figure 1.) The process delivers these benefits by emphasizing health, equity, and community engagement as core values at every step of the planning process.
- Improving data. By bringing health and planning professionals together through a systematic process, HIAs expand the data sources and analytic techniques available and provide a more complete picture of planning decisions’ implications, including potential unintended consequences and opportunities to promote health. For example, by mapping emergency room visits for asthma and neighborhood-level air quality and emissions data, HIA teams can identify and recommend ways to improve respiratory health through better land-use planning. Additionally, by engaging experts with different specializations and community stakeholders, HIA can improve planners’ ability to communicate effectively with multiple audiences using clear, plain language to describe complex relationships between health and planning.
-
Promoting citizen involvement. Planning and HIA professionals share a commitment to engaging diverse stakeholder groups, including those most likely to be affected, and considering how a decision may disproportionately benefit or burden specific population groups such as seniors, children, and low-income communities. The process creates opportunities to leverage the assets of each field. For example, planning professionals often undertake community engagement initiatives as part of their work, and HIAs can complement and strengthen those efforts by helping planners learn about the health priorities of the communities they serve and enabling residents to participate in decisions affecting them.
The city of Minneapolis performed an HIA of the Above the Falls Master Plan, which was drafted to guide redevelopment in a riverfront area, to examine the potential impact on neighborhoods facing significant health disparities and identify how those communities could benefit most from its implementation.10 The HIA team contacted hundreds of community members through an outreach program that included community events, public forums, surveys in English and Spanish, and comment cards to develop recommendations tailored to support the plan’s successful implementation. Among the proposed solutions were programming and activities in the redeveloped riverfront area that engage key groups, including youth, people of color, and people with limited-English proficiency. HIA offers a flexible, complementary tool that planners can use to assess complex issues and strengthen plans, policies, and projects using data and stakeholder input.
- Providing opportunities for cross-sector collaboration. HIAs enable planners, public health professionals, community stakeholders, and decision-makers to work together to ensure that public health is factored into plans, land-use policies, and planning-related actions. The HIA process can build strong relationships and capacity for future partnerships between planning and public health officials and identify opportunities to share resources. For example, an HIA in Oklahoma City strengthened an emerging affiliation between the city’s planning and health departments and contributed to the creation of an ongoing partnership between them and a health-focused position in the planning department.11
- Reframing contentious issues around shared health goals. HIAs can reveal topics of mutual concern among groups with seemingly little common ground. For example, in response to growing controversy between renewable energy advocates and residents living and working near wind turbines, the Oregon Health Authority’s Public Health Division conducted an HIA on wind energy development.12 Representatives from stakeholder groups, including the wind energy industry, utilities, elected officials, local planning and development staff, and community members came together to assess the health effects of wind power generation facilities. The HIA team identified strategies to reduce and resolve conflict in relevant decision-making and made recommendations on locations of turbines relative to homes to help mitigate noise and visual effects.
One County Uses HIA to Inform Farmland Protection Decisions
Kane County, Illinois, which borders Chicago and its suburbs, has a mixture of urban and rural land uses. In 2001, recognizing the need to permanently protect its rich farmland from population growth and increasing development pressure, the county became the first in the state to adopt a farmland protection ordinance. As of the 2007 Agricultural Census, however, Kane County had 192,372 acres of farmland, and only 1,180 acres in vegetable production.* So in 2011, the county considered amendments to the ordinance that were designed to increase total acres dedicated to food production, diversify food crop acres, and provide greater access to fresh local produce by boosting participation under the ordinance among smaller farms that produce fruits, vegetables, and meats and typically sell locally.
The county’s Development and Community Services Department, which oversees land-use planning and agriculture and farmland programs, conducted an HIA in partnership with the Health Department to examine how the proposed amendments could affect the availability of healthy, affordable food and to offer recommendations for protecting and promoting public health. The HIA found that by increasing local production of fruits and vegetables, residents would have access to more local produce and that they would purchase and consume more healthy foods as a result. The economic analysis determined that by shifting 1,000 acres from corn and soybean production to more lucrative and labor-intensive fruit and vegetable production, more than $7 million and 100 jobs would be added to the county’s economy.†
The HIA’s primary recommendation was to develop a new ordinance as a companion to the existing one. This approach would preserve the farmland protection program and its history, which are a point of pride in the county, and create a stand-alone program that, because it would not be tied exclusively to farmland protection, would have more flexibility in funding. Kane County implemented the recommendation, adopting the “Growing for Kane” Ordinance to encourage farmers to grow more fruits and vegetables, enhance the local economy, and make more locally grown nutritious food available to residents. In 2015, Kane County received a Plan4Health grant from the APA to study the feasibility of establishing a food hub—an organization that provides distribution and marketing support to local famers to help reduce their distribution costs and expand their markets—as recommended by the HIA, among other activities. These efforts have the potential to enhance community health by improving residents’ access to healthy, affordable food.
*Kane County Health Department, Growing for Kane Health Impact Assessment Report (2013) accessed September 2015, http://kanehealth.com/PDFs/HIA/KaneCountyHIAReportFinal.pdf.
†Ibid.
The future of HIA in planning
The use of HIAs to inform planning decisions and the resulting evidence base regarding the connections between land-use choices and health has yielded new tools and approaches to integrate consideration of health effects into plans, policies, and projects. For example, the Nashville Area Metropolitan Planning Organization in Tennessee uses scoring criteria for selecting and funding transportation projects that prioritize health promotion.13 Similarly, planners in Meridian Township, Michigan, use a checklist-based tool to evaluate proposed development projects on a range of health criteria such as access to healthy foods, facilitation of social interaction, and alignment with air and water quality standards.14
Because of their role in envisioning and shaping the built, social, and economic environments in communities across the country, planners are at the forefront of efforts to address many of the nation’s most pressing health challenges. Cross-sector collaboration is necessary for solving complex problems, and HIAs facilitate and strengthen relationships among organizations across diverse sectors. HIA and other HIA-inspired approaches will continue to play a critical role in understanding the connections between planning and public health to ensure that health effects are routinely considered as part of the planning process.
About the partnership
In 2014, the Health Impact Project and the American Planning Association (APA) launched a strategic partnership with the goal of expanding the use of HIAs in planning. The partnership supported the development and dissemination of resources to guide the integration of HIA into planning processes. The APA conducted the review of 134 planning HIAs and developed the case study summarized in this brief. Other products arising from this collaboration include an August 2016 report examining how planning HIAs have been used to promote healthy communities, which is available at https://www.planning.org/nationalcenters/health/planninghia. The APA is also creating a toolkit describing how HIAs can be used at different stages of planning, which will be available on the organization’s website in fall 2016.
Endnotes
- National Research Council, Improving Health in the United States: The Role of Health Impact Assessment (Washington: The National Academies Press, 2011), 23-42, http://www.nap.edu/catalog.php?record_id=13229.
- American Planning Association, The State of Health Impact Assessment in Planning (2016), https://planning-org-uploaded-media.s3.amazonaws.com/document/State-of-Health-Impact-Assessment-in-Planning.pdf; APA identified planning HIAs conducted between 2004 and 2014 by searching two databases of HIAs in the United States and conducting outreach to APA members and other stakeholders. APA searched the Health Impact Project database, http://www.pewtrusts.org/en/multimedia/data-visualizations/2015/hia-map, and the UCLA HIA Clearinghouse, http://www.hiaguide.org/hias.
- National Research Council, Improving Health in the United States, 23-42.
- Lauren M. Rossen and Keshia M. Pollack, “Making the Connection Between Zoning and Health Disparities,” Environmental Justice 5, no. 3 (2012): 119-127, http://www.jhsph.edu/research/centers-and-institutes/johns-hopkins-center-for-a-livable-future/_pdf/research/clf_reports/zoning%20health%20disparities%20Rossen Pollack.pdf.
- Health Impact Project, “About Health Impact Assessment,” accessed Oct. 6, 2014, http://www.pewtrusts.org/en/projects/healthimpact-project/health-impact-assessment.
- Ibid; and National Research Council, Improving Health in the United States, 5.
- National Research Council, Improving Health in the United States.
- Plans, policies, and actions were defined as follows: A plan is an official document that sets goals, identifies objectives, and establishes policies that guide future development in a specified geographic area; a policy is an operational process or rule necessary for achieving the goals and objectives set forth in a plan; and an action includes projects or actions undertaken to implement a plan or policy.
- See Andrew L. Dannenberg, et al., “Use of Health Impact Assessment for Transportation Planning: Importance of Transportation Agency Involvement in the Process,” Transportation Research Record no. 2452 (2014): 71-80; and National Center for Healthy Housing and National Housing Conference, A Systematic Review of Health Impact Assessments on Housing Decisions and Guidance for Future Practice (2016), http://www.nchh.org/Portals/0/Contents/Guidance-for-Conducting-HIAs-on-Housing-Decisions.pdf.
- Health Impact Project, “City of Minneapolis Above the Falls Master Plan,” accessed July 13, 2016, http://www.pewtrusts.org/en/multimedia/data-visualizations/2015/hia-map/state/minnesota/city-of-minneapolis-above-the-falls-master-plan.
- John Tankard, City of Oklahoma City Planning Department, personal communication, Aug. 22, 2015; Health Impact Project, “PlanOKC HIA,” accessed April 11, 2016, http://www.pewtrusts.org/en/multimedia/data-visualizations/2015/hia-map/state/oklahoma/planokchia.
- Oregon Health Authority, “Wind Energy Facility Siting HIA,” accessed July 14, 2016, https://public.health.oregon.gov/HealthyEnvironments/TrackingAssessment/ HealthImpactAssessment/Pages/windenergy.aspx.
- Nashville Area Metropolitan Planning Organization, “Health & Well Being,” accessed March 5, 2016, http://www.nashvillempo.org/regional_plan/health/.
- Charter Township of Meridian, “Charter Township of Meridian Health Impact Assessment,” accessed March 7, 2016, http://advance.captus.com/planning/hia2/pdf/Module2/ InghamCountyMeridanTownshipChecklist.pdf.






