Quality Monitoring, Evolving Since Nineteenth Century, Can Improve Prison Health Care
Pew report identifies 35 states with a monitoring system
This is the seventh analysis in a series examining how health care is funded and delivered in state-run prisons, as well as how care continuity is facilitated upon release.
The health care that prisons provide affects more than simply the well-being of incarcerated people. Inadequate treatment for infectious diseases and behavioral health conditions, for example, can undermine efforts to strengthen public health and safety in the communities to which individuals return. Assessments of what taxpayers are getting for their prison health care dollars and how that compares to other states depends on an evaluation of the care provided.
Nevertheless, policymakers and administrators do not always have the information they need—or regularly use what they do have—to proactively identify shortcomings and make improvements to care quality, risking ill-informed uses of scarce resources and missed opportunities.
A first-of-its-kind report by The Pew Charitable Trusts details whether and how states monitor the quality of care they provide.
Origin of quality monitoring
In 1847, Ignaz Semmelweis, a physician practicing in Vienna General Hospital’s maternity clinic, faced a vexing question: Why were so many new mothers dying from infections? After several unsuccessful interventions, he identified the answer: scant handwashing by doctors who performed autopsies when they weren’t delivering babies. Clean hands and instruments produced a dramatic reduction in cases of puerperal fever. This was perhaps the first instance of rigorous health care quality monitoring and improvement.
Half a century later, Ernest Codman, a pioneering surgeon in Boston, began advocating for an “end results” system that would track and make public the outcomes of care. He urged doctors to conduct follow-up examinations and produce performance data that could be standardized and published by hospitals. These data would help identify opportunities for enhancements and increase accountability by arming patients with comparable information. Through these efforts, Codman launched the modern movement to monitor and improve health care quality.
Quality monitoring in the U.S. today
Recent decades have seen a drive to develop and implement measures and systems for monitoring quality, largely in response to evidence of disparities and deficiencies among providers. Several bodies—including the National Committee for Quality Assurance, the National Quality Forum, and the Centers for Medicare & Medicaid Services—have provided guidance. Today, most health insurance providers undergo annual quality measurement and public reporting of results.
The Institute of Medicine defines quality of care as “the degree to which health services for individuals and populations increase the likelihood of desired health outcomes and are consistent with current professional knowledge.” The institute separates care quality into six dimensions: safety, effectiveness, patient-centeredness, timeliness, efficiency, and equity.
Within this framework, each dimension can be evaluated based on structure, process, and outcome. Structural components represent relatively fixed inputs of care, such as the number of beds. Process measures relate to the actions of providers and their interactions with patients, while outcomes pertain to near- and long-term effects of providing care.
Pew research on quality monitoring
As health care quality measurement and monitoring have matured in the community, some state prison health care systems—alongside their colleagues in state Medicaid and employee health insurance agencies—have begun integrating such activities into their operations. Still, there are no uniform quality-of-care standards for correctional systems and facilities, or mechanisms for reporting comparable performance data. Little systematic information exists about state actions and actual outcomes.
Pew studied operations in the 50 states to begin clarifying these points. This research offers practical information and insights that decision-makers can use to help optimize policies and programs in the service of incarcerated individuals, state residents, and taxpayers.
Thirty-five states reported that they operated a prison health care quality monitoring system in fiscal year 2016. Of these, however, only six—Florida, Nebraska, Nevada, New Jersey, New York, and Texas—indicated that they required quality monitoring and built in regular opportunities to incorporate the findings into decision-making and legislative oversight. Such practices can help define priorities, bolster consistency amid personnel changes, and ensure that objectives are met.
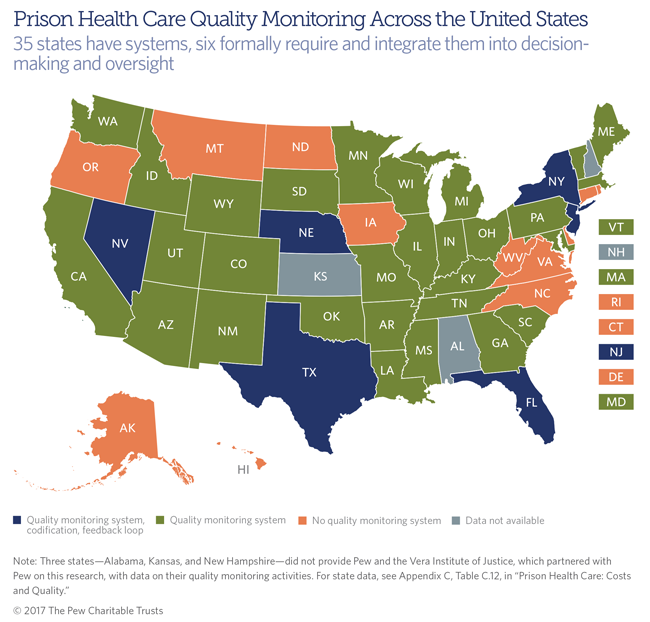
The 35 states’ systems varied significantly with respect to objectives, scope and focus, and whether and how the systems are used to inform spending and management decisions.
States without quality monitoring systems reported engaging in a wide range of related activities, including regular audits of practices and protocols, inmate grievance investigations, and mortality reviews. But a majority agreed or strongly agreed that establishing such a system is necessary to achieve at least an adequate level of quality, improve the quality of care provided, and improve the states’ understanding of the value of their prison health care spending.
“I can tell the Legislature exactly where every penny went. … I can tell them where the buck went,” said Steven Shelton, former chief medical officer of the Oregon Department of Corrections. “But without outcome and quality monitoring systems, I can’t tell them what they get for that buck.”
Matt McKillop is an officer with the states’ fiscal health project of The Pew Charitable Trusts.