Could Efforts to Fight the Coronavirus Lead to Overuse of Antibiotics?
Study shows more than half of hospitalized COVID-19 patients in U.S. received antibiotics in pandemic’s first six months
Overview
For years, leading public health and national security experts have sounded the alarm about the growing threat of antibiotic-resistant bacteria. The more antibiotics are used, the faster that bacteria evolve to resist them, giving rise to so-called “superbugs”—bacteria that are extremely difficult or impossible to treat with existing drugs. Minimizing inappropriate prescribing of antibiotics is critical to slow the spread of these stubborn, sometimes deadly pathogens.
As health care providers work to combat the coronavirus, hospital officials have anecdotally reported that it is common for COVID-19 patients to be prescribed antibiotics. Even though antibiotics won’t cure viruses, including COVID-19, physicians concerned about secondary bacterial infections may nevertheless prescribe antibiotics to COVID-19 patients, sometimes before a bacterial infection is confirmed.
There is limited quantitative data describing to what extent people hospitalized with COVID-19 are receiving antibiotics, and whether these patients had a bacterial infection. To better understand these aspects of the pandemic, The Pew Charitable Trusts conducted one of the largest studies to date of antibiotic use in hospitalized COVID-19 patients, using IBM Watson Health’s electronic health records database to capture data about approximately 5,000 patients and nearly 6,000 hospital admissions from February through July 2020. This study assessed the frequency of bacterial infections and antibiotic prescribing patterns in hospitalized patients diagnosed with COVID-19 in the U.S.
Key findings:
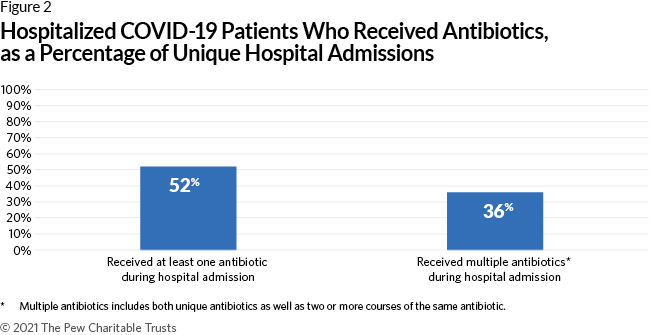
- A majority of COVID-19 hospital admissions led to one or more antibiotics being given to patients. Over half of the COVID-19 hospital admissions captured in this study (52%) resulted in at least one antibiotic prescription, with 36% of admissions resulting in a patient being prescribed multiple antibiotics during hospitalization.
- Compared to the number of hospitalized COVID-19 patients who received antibiotics, far fewer patients admitted for COVID-19 had common bacterial infections. Only 20% of those admitted with the virus were diagnosed with suspected or confirmed bacterial pneumonia, and 9% were diagnosed with a community acquired urinary tract infection.
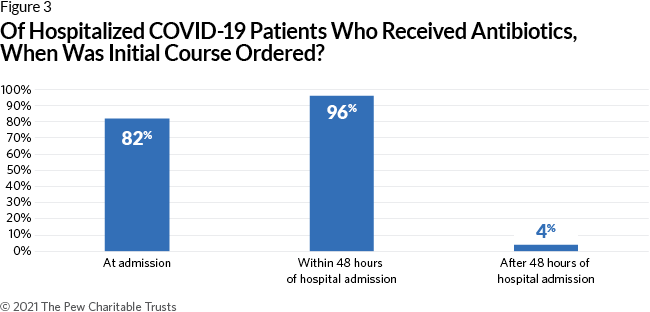
- In most cases, antibiotics were given to COVID-19 patients prior to confirmation of a bacterial infection. In 96% of admissions for patients diagnosed with COVID-19 in which an antibiotic was prescribed, the patient received the first antibiotic at admission or within the first 48 hours of hospitalization. It typically takes at least 48 hours to confirm a bacterial infection, so it appears that physicians frequently prescribed antibiotics empirically, i.e., before confirmation of a known bacterial infection.
The findings strongly suggest that overprescribing of antibiotics occurred during the first six months of the pandemic. Although it was not possible from this study to determine the proportion of antibiotic treatments that were inappropriate, the disparity between the percentage of patients who received antibiotics and those who were diagnosed with bacterial infections indicates that some patients received antibiotics unnecessarily. This unnecessary prescribing was likely driven by factors such as challenges in differentiating between COVID-19 pneumonia and bacterial pneumonia, concerns that patients might have bacterial co-infections, and limited understanding and experience in managing COVID-19 patients during the early phases of the pandemic.
Antibiotic stewardship programs—which are required for most hospitals by regulatory and accreditation organizations—aim to ensure that antibiotics are prescribed only for known or suspected bacterial infections, and that the right antibiotic is prescribed at the appropriate dose and duration of therapy. As such, these programs can—and should—play a critical role in helping health care providers reduce inappropriate prescribing associated with COVID-19. It is essential that stewardship programs have the resources necessary to ensure that physicians have access to information and guidance needed to make the best antibiotic treatment decisions for their patients and to improve prescribing.
Background on study population
In total, the study includes 5,838 unique hospital admissions, representing 4,980 patients. Some patients were admitted more than once and may have received antibiotics during more than one hospital stay. (See “Methodology” for additional information.) The study examined antibiotic prescribing and was not designed to be a nationally representative sample but does represent a large population distributed across the United States. All findings presented in this issue brief are based on the unique admissions data.
Table 1 highlights key characteristics of this study’s population. Nearly half of admissions were patients ages 56 years and older, and 52% of admissions were female. Most admissions occurred in the Midwest (84%), followed by the South (14%). Additionally, White and Black patients each accounted for 40% of admissions, which reflects findings from other studies that show Black patients are overrepresented among hospitalized COVID-19 patients compared to their percentage of the country’s overall population.1 Around 40% of admissions occurred in July, indicating that this study’s population primarily shows treatment patterns prevalent in the summer of 2020, following the initial months of the pandemic.
Fifty-nine percent of admissions lasted one to three days, with an average length of stay of just over five days. In 9% of admissions, the patient required the use of a ventilator or intubation, and in 5% of the admissions, the patient died.
Comprehensive data on U.S. hospitalized COVID-19 patients remains limited, making it difficult to identify how the population assessed for this study compares to national statistics. However, information from other research indicates that this study’s population may skew younger than the broader population of hospitalized COVID-19 patients.2 Additionally, the patients captured in this study experienced a relatively short length of hospitalization and a low mortality rate compared to other studies of hospitalized COVID-19 patients in the U.S.3 These differences could mean that this study population was relatively healthier or experienced less severe illness than the broader U.S. hospitalized COVID-19 population.
Table 1
Demographic and Admission Characteristics of Patient Population (N=5,838 unique hospital admissions)
| Age | Unique admissions | Percentage |
|---|---|---|
| 0-17 years old | 102 | 2% |
| 18-34 years old | 1,101 | 19% |
| 35-45 years old | 794 | 14% |
| 46-55 years old | 930 | 16% |
| 56-65 years old | 1,132 | 19% |
| 66-75 years old | 890 | 15% |
| Older than 75 years old | 866 | 15% |
| Missing | 23 | <1% |
| Gender | Unique admissions | Percentage |
|---|---|---|
| Male | 2,794 | 48% |
| Female | 3,044 | 52% |
| Race/ethnicity | Unique admissions | Percentage |
|---|---|---|
| White, non-Hispanic | 2,308 | 40% |
| Black, non-Hispanic | 2,318 | 40% |
| Hispanic | 597 | 10% |
| Asian, non-Hispanic | 77 | 1% |
| Other | 165 | 3% |
| Unknown | 373 | 6% |
| Geographic region | Unique admissions | Percentage |
|---|---|---|
| Northeast | 70 | 1% |
| Midwest | 4,880 | 84% |
| South | 840 | 14% |
| West | * | 0% |
| Missing or Other (including Puerto Rico) | 40 | 1% |
| Month of hospital admission | Unique admissions | Percentage |
|---|---|---|
| February | * | 0% |
| March | 380 | 7% |
| April | 1,000 | 17% |
| May | 1,100 | 19% |
| June | 1,030 | 18% |
| July | 2,320 | 40% |
| Length of hospital admission | Unique admissions | Percentage |
|---|---|---|
| 1-3 days | 3,443 | 59% |
| 4+ days | 2,395 | 41% |
| Required ventilation or intubation | Unique admissions | Percentage |
|---|---|---|
| Yes | 502 | 9% |
| Mortality | ||
| Deceased | 285 | 5% |
| Non-deceased | 5,553 | 95% |
* Unable to report results due to cell size of <11 admissions. The other categories associated with this characteristic have been rounded to ensure masking.
© 2021 The Pew Charitable Trusts
Bacterial infections in hospitalized COVID-19 patients
Bacterial infections can occur simultaneously in patients diagnosed with viral infections such as COVID-19 and can complicate the patient’s illness and the appropriate course of treatment. For the purposes of this study, the researchers assessed the occurrence of bacterial co-infections by (1) identifying bacterial infections based on diagnosis coding and (2) identifying bacterial infections through microbiology testing that confirmed the presence of bacteria in culture samples (Figure 1). Although each approach has limitations that could lead to over- or underestimations, both were used to provide insight into the presence of bacterial infections among COVID-19 patients. (See “Limitations” for additional information.)
Using diagnosis codes, researchers evaluated the occurrence of bacterial pneumonia, urinary tract infections, ventilator-associated pneumonia, and bloodstream infections. In about 20% of COVID-19 admissions, the patient was diagnosed with bacterial pneumonia, almost of all which were cases of community-acquired pneumonia. (See “Methodology” for the study’s definition of community-acquired infections.) In 9% of COVID-19 admissions, patients were diagnosed with community-acquired urinary tract infections. The study was not able to determine the extent to which there is overlap between patients with these two types of infections. Occurrences of bloodstream infections and ventilator-associated pneumonia were too infrequent to report.
When microbiology testing results were used to identify bacterial infections, only about 7% of COVID-19 admissions were found to have positive bacterial culture results from respiratory, blood, and urine samples. Due to limitations in the data, the study was not able to differentiate percentages between specific sample types.
Although the analyses using diagnosis codes and microbiology testing showed some variability in bacterial infection rates, the data shows that bacterial co-infections are occurring within hospitalized COVID-19 patients but likely at small percentages.
Antibiotic prescribing for hospitalized COVID-19 patients
Within the study population, over half of admissions (52%) resulted in at least one antibiotic being prescribed during a patient’s hospitalization (Figure 2). Thirty-six percent of admissions resulted in multiple antibiotics being prescribed to treat patients. Additionally, most patients received their first antibiotic at admission or within the first 48 hours of hospitalization (96% of admissions where an antibiotic was prescribed; Figure 3). These findings may indicate that antibiotics are being prescribed empirically, meaning before confirmation of a known bacterial infection. This is because most cultures—which can confirm a bacterial infection beyond a clinical diagnosis—often take 48 hours to provide results. Although empiric prescribing can help to ensure that patients with an active infection receive antibiotics in a timely manner, it may also expose patients to antibiotics unnecessarily.
The analysis also found that few patients received additional antibiotics after 48 hours. Only 15% of admissions included in this study (28% of admissions where at least one antibiotic was prescribed) resulted in an antibiotic course prescribed within the first 48 hours of admission and another course ordered after the first 48 hours. Although a majority of admissions resulted in antibiotic prescribing, it appears that fewer antibiotics are being prescribed after physicians receive additional information on whether a patient has a bacterial infection.
A key aspect of antibiotic stewardship programs in hospitals is de-escalation: ensuring that patients who were started on antibiotics are taken off them if culture results show they don’t have a bacterial infection. The finding that fewer patients are receiving additional antibiotics after 48 hours may indicate that antibiotic stewardship efforts are working during the COVID-19 pandemic to minimize inappropriate antibiotic prescribing.
Patient factors and hospitalization characteristics associated with antibiotic prescribing
The study also examined patient factors—such as clinical characteristics—according to whether an antibiotic was prescribed during the hospital admission. Clinical diagnosis of a bacterial infection was clearly associated with antibiotic prescribing (see Figure 4). Among COVID-19 admissions where antibiotics were prescribed, 33% had a diagnosis of community-acquired bacterial pneumonia. Among COVID-19 admissions where antibiotics were not prescribed, only 4% had a diagnosis of community-acquired bacterial pneumonia. Similarly, among COVID-19 admissions where antibiotics were prescribed, 14% were diagnosed with a community-acquired urinary tract infection, compared to only 4% of admissions where an antibiotic was not prescribed.
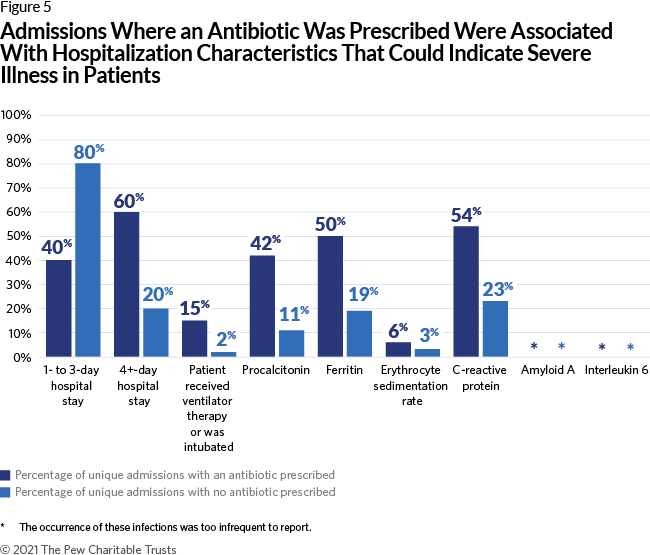
Other elements associated with antibiotic prescribing were those that could indicate severity of disease for a patient (see Figure 5). Specifically, patients who received antibiotics were more likely to have a longer hospitalization: Sixty percent of admissions with an antibiotic prescription were for hospitalizations of four or more days, while only 20% of admissions without an antibiotic prescribed lasted four or more days. Additionally, the average length of stay for admissions where patients received antibiotics was nearly eight days, versus approximately three days when the patient did not receive antibiotics. Fifteen percent of admissions with an antibiotic prescription were associated with the patient being placed on a ventilator or intubated, while only 2% of admissions without an antibiotic were associated with the same procedure. Patients who received antibiotics were more likely to have inflammatory markers that could indicate an active infection that might necessitate antibiotic use. (See “Methodology” for information on how inflammatory markers were identified.) Although these markers cannot distinguish between a bacterial or viral infection, they usually reflect a higher level of severity of disease in a patient and a potentially appropriate indication for empiric antibiotic treatment.
Antibiotic selection
The study showed that the antibiotics most commonly prescribed to treat hospitalized COVID-19 patients were:
(1) azithromycin (50% of admissions where an antibiotic was prescribed), (2) ceftriaxone (42%), (3) vancomycin (25%), and (4) piperacillin/tazobactam (23%). Although researchers were unable to assess the appropriateness of the use of these specific types of antibiotics, it was likely driven by empiric prescribing for community-acquired bacterial infections as all four antibiotics are commonly recommended to treat such infections (including bacterial pneumonia).4 Earlier in the pandemic, azithromycin was combined with antimalarial drugs chloroquine and hydroxychloroquine as a potential treatment for patients with COVID-19, which also could account for the high level of use found in this study.5
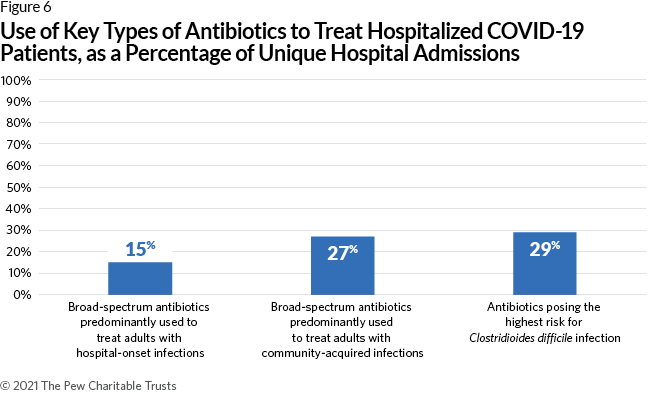
The study also evaluated prescribing practices for key types of antibiotics, such as broad-spectrum antibiotics (i.e., antibiotics that target a wide range of bacterial pathogens and that are known to accelerate the development of resistance) and those that pose the highest risk of causing a Clostridioides difficile (C. difficile) infection, which can cause life-threatening diarrhea (Figure 6). In 15% percent of admissions, patients were given a broad-spectrum antibiotic commonly used to treat adults with hospital-onset infections, and in 27% of admissions, patients were prescribed a broad-spectrum antibiotic commonly used to treat adults with community-acquired infections. Additionally, 29% of admissions resulted in an antibiotic within the group known to pose a high risk for C. difficile. Antibiotic stewardship programs often emphasize caution when prescribing these types of antibiotics in order to minimize the development of resistance or the occurrence of adverse patient outcomes such as C. difficile.
Implications for combating antibiotic resistance during the COVID-19 pandemic and beyond
Well before the pandemic began, public health authorities warned that antibiotic resistance was an urgent public health threat. The rise of resistant pathogens over time is inevitable, as bacteria evolve to resist antibiotics, and researchers must develop novel drugs to attack infectious agents. However, in recent decades the discovery and development of new antibiotics has slowed to a trickle, as large pharmaceutical companies have left the field. Public health authorities around the world are seeking ways to spur new development.
The lack of new drugs in the development pipeline has made the role of antibiotic stewardship programs even more important; with few new drugs on the horizon, preserving the effectiveness of existing drugs is crucial.
This study does indicate that existing stewardship efforts may be having a positive effect on efforts to ensure appropriate antibiotic prescribing: The data showed that most patients who were given antibiotics early on in their hospitalization did not receive additional courses after 48 hours. This demonstrates that de-escalation— a key aspect of antibiotic stewardship programs in hospitals—is likely being implemented and helping to reduce inappropriate prescribing during the pandemic.
However, the significant amount of antibiotic use for COVID-19 patients and the increased hospitalization rates of the pandemic call for devoting resources to strengthen stewardship programs. Activities such programs can undertake to support COVID-19 response efforts in hospitals include:
- Working to identify drivers of inappropriate antibiotic prescribing—such as the difficulty in differentiating coronavirus-related pneumonia and bacterial pneumonia—and developing clinical guidelines and treatment protocols to aid in management of COVID-19 patients.
- Helping to ensure that antibiotics are de-escalated when additional clinical information (such as culture results) is available, such as discontinuing antibiotics once a patient is confirmed to have COVID-19 and the likelihood of a secondary bacterial infection is low.
- Providing guidance to physicians on appropriate antibiotic selection for treating COVID-19 patients, including directing physicians to prescribe narrow-spectrum antibiotics when appropriate and minimizing the use of antibiotics known to cause adverse events such as C. difficile infections.
The use of antibiotics during this pandemic has the potential to impede progress made in recent years to combat antibiotic resistance in the U.S.6 New types of antibiotics are urgently needed to defeat rapidly evolving bacteria. The continued expansion of antibiotic stewardship efforts across health care settings will be needed to ensure that these critical therapies remain effective in the future.
Methodology
This analysis was conducted using IBM Watson Health’s Explorys electronic health record database. All inpatient stays with an admission date between Feb. 1, 2020, and July 31, 2020, and discharged by Sept. 7, 2020 (the date of the final data pull), were reviewed and included if they met study requirements. Emergency department only stays and observation stays were not included. The inclusion criteria were:
- A patient needed to have been diagnosed with COVID-19 (identified using the ICD-10 diagnostic code for COVID-19 or through a positive laboratory test) up to 14 days before hospital admission or three days after hospital admission. For patients identified through a positive laboratory test, the date is based onthe day the test was administered, not when results were received. The date of hospital admission was counted as day zero.
- A patient needed to have information on prescription drug orders associated with their inpatient stay. This was required in order to ensure that Explorys was able to capture any antibiotic prescribing associated with that patient’s hospital stay.
Data was provided for each unique inpatient admission. If an inpatient admission had a discharge date that was the same day or up to two days before a subsequent inpatient admission, this data was grouped together as a single admission. Overall, there were 5,838 unique hospital admissions included in this analysis, representing 4,980 patients (some patients had multiple admissions during the study period).
The occurrence of the bacterial infections included in this analysis—bacterial pneumonia, ventilator-associated pneumonia, bloodstream infections, and urinary tract infections—were identified using ICD-10 diagnosis codes. A bacterial infection was considered community-acquired if it was diagnosed within 48 hours of hospitalization (date of admission counted as day zero, so any infection that was diagnosed on day zero, one, or two). Any infection diagnosed after 48 hours was considered associated with the hospitalization. Positive bacterial culture results were identified by the presence of susceptibility testing results associated with a given hospital admission. The researchers only evaluated culture results for respiratory, blood, and urine samples.
The antibiotics included in this analysis were based on the list of antibiotics reported to the Centers for Disease Control and Prevention’s National Healthcare Safety Network through the Antimicrobial Use (AU) Option. The researchers were unable to fully control for route of administration. Similar to the bacterial infection analysis, an antibiotic was considered to have been prescribed within the first 48 hours of a hospital admission if the order occurred on day zero, one, or two of admission. Antibiotics were grouped into the following categories based on guidance provided for the AU Option: (1) broad-spectrum antibiotics predominantly used to treat hospital-onset infections, (2) broad-spectrum antibiotics predominantly used to treat community-acquired infections, and (3) antibiotics posing the highest risk for C. difficile infections.
Patient demographics were identified based on the most recent non-missing characteristics captured within the Explorys database. Race and ethnicity were combined into one variable. Geographic region was defined based on the four U.S. Census regions. Whether a patient required use of a ventilator or intubation during their admission was identified using SNOMED codes, which are standardized codes for medical terminology used for analyzing electronic health record data. The presence of positive test results for the following inflammatory markers was evaluated in the database: procalcitonin, ferritin, erythrocyte sedimentation rate, C-reactive protein, amyloid A, and interleukin 6. Tests for these markers were identified using Logical Observation Identifiers Names and Codes (LOINC). Patients were considered positive for an inflammatory marker if the result for the patient was above the “normal” or “reference” ranges defined by the laboratory performing the test.
All programming was completed by the IBM Watson team using SQL and Python on a secure server.
Limitations
This analysis has a number of limitations. First, Explorys contributors are more likely to be located in the Midwest and Southern regions of the United States, so findings may not be representative of the U.S. as a whole. Second, Explorys only captures data provided by physicians who report into the Explorys database. It may not include a full clinical picture of a patient if that individual is also treated by a physician who does not report to Explorys. Third, while some electronic health records indicate that a laboratory test has been ordered or a prescription has been written, that does not necessarily mean that the test was given or prescription was filled. This limitation was mitigated in the analysis for laboratory tests by requiring the presence of a test result to show that the test was administered. Fourth, the researchers were unable to link the timing of an antibiotic prescription to a clinical diagnosis or laboratory test result, limiting the ability to link an antibiotic prescription with specific clinical decision-making.
The two approaches used for identifying bacterial infections in this study—use of diagnosis codes and microbiology testing—have limitations. Relying on diagnosis coding may overestimate the occurrence of these infections because it relies on medical record documentation that can include not only confirmed cases of bacterial infections, but suspected cases based on a physician’s clinical judgment. However, relying on positive bacterial culture results also has limitations. Physicians may be more limited in their ability to obtain respiratory samples from COVID-19 patients due to infection control protocols, potentially leading to an underestimate of the occurrence of bacterial infections.7 Additionally, susceptibility testing may not be conducted for certain bacterial pathogens, such as H. influenzae. In contrast, reliance on susceptibility test results may also overestimate the occurrence of bacterial infections for certain cultures, such as those acquired from urine samples.8
Endnotes
- V.M. Vaughn et al., “Empiric Antibacterial Therapy and Community-Onset Bacterial Co-Infection in Patients Hospitalized With COVID-19: A Multi-Hospital Cohort Study,” Clinical Infectious Diseases (2020), https://doi.org/10.1093/cid/ciaa1239; S. Garg et al., “Hospitalization Rates and Characteristics of Patients Hospitalized With Laboratory-Confirmed Coronavirus Disease 2019—COVID-Net, 14 States, March 1-30, 2020,” Morbidity and Mortality Weekly Report 69, no. 15 (2020): 458-64, http://dx.doi.org/10.15585/mmwr.mm6915e3; United States Census Bureau, “QuickFacts,” accessed March 3, 2021, https://www.census.gov/quickfacts/fact/table/US/RHI225219.
- M.W. Fried et al., “Patient Characteristics and Outcomes of 11,721 Patients With Coronavirus Disease 2019 (COVID-19) Hospitalized Across the United States,” Clinical Infectious Diseases (2020), https://doi.org/10.1093/cid/ciaa1268; Garg et al., “Hospitalization Rates.”
- Fried et al., “Patient Characteristics and Outcomes”; J.A.W. Gold et al., “Characteristics and Clinical Outcomes of Adult Patients Hospitalized with COVID-19—Georgia, March 2020,” Morbidity and Mortality Weekly Report 69, no. 18 (2020): 545-50, http://dx.doi. org/10.15585/mmwr.mm6918e1; L.C. Myers et al., “Characteristics of Hospitalized Adults With COVID-19 in an Integrated Health Care System in California,” JAMA 323, no. 21 (2020): 2195-98, https://doi.org/10.1001/jama.2020.7202; Vaughn et al., “Empiric Antibacterial Therapy.”
- J.P. Metlay et al., “Diagnosis and Treatment of Adults With Community-Acquired Pneumonia: An Official Clinical Practice Guideline of the American Thoracic Society and Infectious Diseases Society of America,” American Journal of Respiratory and Critical Care Medicine 200, no. 7 (2019): e45-e67, https://www.atsjournals.org/doi/abs/10.1164/rccm.201908-1581ST.
- National Institutes of Health, “Chloroquine or Hydroxychloroquine With or Without Azithromycin,” accessed Nov. 20, 2020, https://www.covid19treatmentguidelines.nih.gov/antiviral-therapy/chloroquine-or-hydroxychloroquine-with-or-without-azithromycin/.
- Centers for Disease Control and Prevention, “Antibiotic Resistance Threats in the United States, 2019” (2019), https://www.cdc.gov/drugresistance/pdf/threats-report/2019-ar-threats-report-508.pdf.
- Vaughn et al., “Empiric Antibacterial Therapy.”
- L.A. Petty et al., “Risk Factors and Outcomes Associated With Treatment of Asymptomatic Bacteriuria in Hospitalized Patients,” JAMA Internal Medicine 179, no. 11 (2019): 1519-27, https://doi.org/10.1001/jamainternmed.2019.2871.