A Look at the Evolution of the Virus That Causes COVID-19
Pew scholar and evolutionary microbiologist discusses the emergence of virus variants
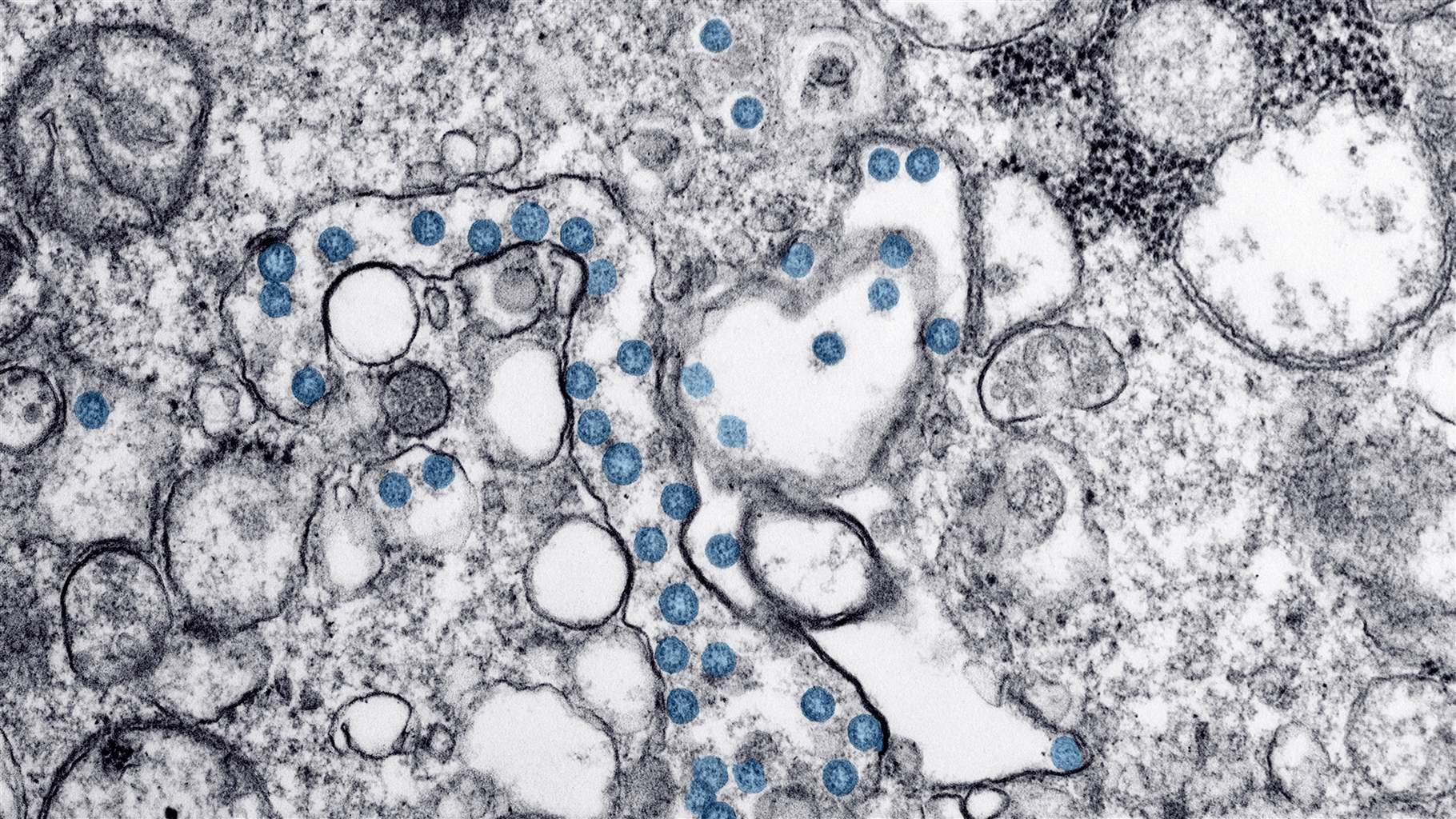
Since the initial outbreak of SARS-CoV-2, the virus that causes COVID-19, the continued emergence of new variants has challenged scientists and forced many people worldwide to adapt to what feels like an ever-changing virus.
The World Health Organization monitors variants and has classified several different “variants of concern”—the most recent of which, omicron, has driven a global surge in COVID-19 cases. Variants form when mutations occur in a virus’ genetic code. SARS-CoV-2 changes as it spreads, creating new strains that can behave differently than the original virus. Some variants can lead to symptoms that are more severe than those caused by other variants; some lead to symptoms that are less severe. Some variants are more easily transmissible than others; some demand new approaches to prevention and treatment.
This interview with Michael Baym, Ph.D., an assistant professor of biomedical informatics at Harvard University and a 2020 Pew biomedical scholar, has been edited for length and clarity.
Q: What causes the creation of new virus variants?
A: We’re seeing a textbook example of evolution in real time. As the virus spreads around the world, it replicates billions of times. Rare mistakes in replication introduce mutations, the majority of which either do nothing or harm the virus. However, very rare combinations of mutations can allow the virus to spread much faster (such as the alpha and delta variants), evade the immunity from previous infections (beta and gamma variants), or both (omicron variant). These mutations either allow the virus to directly outcompete its ancestor—or, as we’re seeing with omicron, infect people who were largely immune to previous strains.
Q: After two years, why is SARS-CoV-2 still changing—and new variants emerging?
A: There’s an interesting question lurking in here: Since there are so many infections, individual viral mutations are happening all the time. If it was a simple progression of mutation after mutation, with each form of the virus gaining the ability to better replicate, then we should expect the same pattern of mutations emerging simultaneously everywhere, right? But we don’t see this. So more likely what’s happening is that the virus is taking advantage of different environments—for example, remaining within a single patient for a long period or jumping to an animal host—and then emerging after adapting. This allows the virus to get around any potential tradeoffs between evasion of the immune system and being able to spread more effectively by adapting to one and then the other, instead of both simultaneously. To me, these scenarios are the most plausible reason for why variants seem to appear with many new mutations at the same time, and why we aren’t seeing intermediate versions of the virus between the variants and their ancestors.
Q: Should we expect this pattern of emerging variants to continue?
A: I really don’t see why we wouldn’t. With unprecedented numbers of infections being reported worldwide, the virus has more chances than it needs to mutate, to jump species, or to infect long-term. We like to draw pictures of evolution as climbing a mountain of fitness, and so there’s some notion of a peak, where it can’t evolve any further. But that isn’t what’s happening here: Our immune responses are evolving along with the virus, shifting the landscape. While this variant or the next may indeed be the last, there’s no theoretical reason why it has to be.
Q: What sets omicron apart from previous variants?
A: To me, one of the strangest and most alarming features of omicron is that it is not a descendant of delta. This fall, as delta swept the world, replacing all other variants everywhere, it seemed inevitable that the next variant would emerge from it. How could it not? Every other variant was displaced. Omicron, however, diverged sometime in mid-2020. So how many more time bombs like omicron are already set, waiting to emerge each day with every million new infections?
Q: What can we do to help manage the virus’s evolution?
A: As long as the virus continues to spread, it will continue to evolve. So, our approach needs to be twofold: We have to reduce the number of infections, and monitor the circulating virus so that we can respond quickly and effectively when new variants arise.
Q: How do vaccines help?
A: They help immediately by reducing the number of infections. But even when they’re not matched well enough to stop infection entirely, vaccines can decrease the chance of a long-term infection—which potentially breaks the chain of events that would lead to a new variant.
Q: You also mentioned monitoring.
A: Monitoring for new variants is critical. The roughly 100 days from discovery of a new strain to distribution of a new mRNA vaccine is nothing short of remarkable—but, as we’ve seen with omicron, that may still not be fast enough. Every additional week of advance notice of a dangerous new variant buys us that much more time to make, test, and distribute a vaccine. This rapid development cycle allows us for the first time in human history to coevolve our vaccines in real time alongside the virus.
Q: It seems that the scientific response in general has been, to borrow your phrase, “nothing short of remarkable.”
A: I want to acknowledge the important work on the SARS-CoV-2 pandemic being done by many, including in the community of Pew scholars. Whether making computational predictions to advise governments, treating patients, or even serving as a local community expert called upon to bring some clarity amidst the haze of changing information, it’s been heartening to see so many scientists rise to the occasion.
Q: What does the future look like?
A: I wouldn’t trust any prediction right now. Flu strains that descended from the 1918 pandemic remain with us today, and other types of coronaviruses that cause the common cold—known as seasonal coronaviruses—continue to circulate. The virus that causes COVID-19 may well be with us for the remainder of human existence, so the question to me really is: How do we best live in a world with this virus?
By the end of the omicron wave, most of the world’s population will, by infection, vaccination, or both, have some immunity to the virus. That should make it that much harder for the next variant to spread, and should also make the next variant’s consequences less severe. Together with effective antiviral medications, I see COVID-19 eventually becoming a manageable infection. I personally don’t expect us to need annual boosters for new strains (like we do with influenza), and I expect that as our ability to prevent and treat infections increases, the kind of societal restrictions we’ve seen in the past two years will become more costly than beneficial. But then again, this virus has surprised us before—so who’s to say it won’t do so again?