Diagnostic Tests Not Reviewed by FDA Present Growing Risks to Patients
Congress should pass reforms to ensure accuracy, reliability, and quality
To get well and stay well, you first need to know what’s making you sick. That’s why blood, saliva, and other in vitro diagnostics (IVDs) are so critical to modern medicine. According to new research commissioned by The Pew Charitable Trusts, about 3.3 billion of these tests are run each year to monitor health, detect the presence of or risk for myriad diseases and conditions, and guide treatment. Although the Food and Drug Administration actively regulates many tests for safety and effectiveness, it does not review a significant but unknown number of diagnostics referred to as lab-developed tests (LDTs).
To ensure the public has access to safe, reliable, accurate, and innovative diagnostics, Congress should pass legislation that would increase the transparency of the market and authorize FDA to review them based on their risks to patients.
Insufficient transparency
LDTs have been developed for a wide range of conditions, including infectious diseases such as COVID-19, as well as different types of cancer. Because LDTs are not centrally registered or tracked, however, no one knows precisely how many of them are on the market, when and why they are used, or how their performance compares to FDA-reviewed diagnostics. Insurance claims and electronic health records do not distinguish between LDTs and FDA-reviewed diagnostics, and there are no comprehensive databases of all LDTs in use. And in a series of interviews that Pew commissioned, even seasoned clinical lab managers demonstrated confusion over what exactly constitutes an LDT.
Outdated rules
FDA provides several layers of oversight for diagnostics that are mass produced and marketed for use in labs across the U.S. and around the world. However, it does not review or approve LDTs, which are developed and used in a single lab. Instead, the Centers for Medicare & Medicaid Services (CMS) regulates the labs in which LDTs are created. But CMS has only partial oversight over those tests. (See Figure 1.)
Figure 1
Key Public Health Protections Missing From Federal Oversight of Lab-Developed Tests
Despite similarities, LDTs and FDA-reviewed tests are not held to the same standards
| FDA-reviewed in vitro diagnostics | Lab-developed tests | |
|---|---|---|
| Moderate- and high-risk tests are reviewed externally before use on patients | Yes | No |
| Tests are registered in a public database | Yes | No |
| Public reporting of adverse events related to an incorrect test result is mandatory | Yes | No |
| Product labeling is reviewed and approved to ensure that it is comprehensive and accurate | Yes | No |
| Marketing claims must be supported by evidence and approved before use in a clinical setting | Yes | No |
| Oversight body is able to recall faulty tests | Yes | No |
© The Pew Charitable Trusts 2021
This approach to oversight was more appropriate in 1976, when Congress first granted FDA authority over medical devices; most LDTs at that time were relatively simple or were used as customized tests for rare conditions that could not be detected with commercially available diagnostics. According to Pew research, however, LDTs are being used today for different reasons and in new ways that increase the risk of faulty tests. For example:
- LDTs are increasingly used to identify and manage the treatment of more common and serious diseases, and where the risks posed by inaccurate results are dangerously high, such as for cancer, prenatal conditions, and genetic diseases.
- Once limited to patients near one lab, LDTs can now reach millions of consumers across the country, thanks to the internet, rapid shipping, and advances in at-home specimen collection.
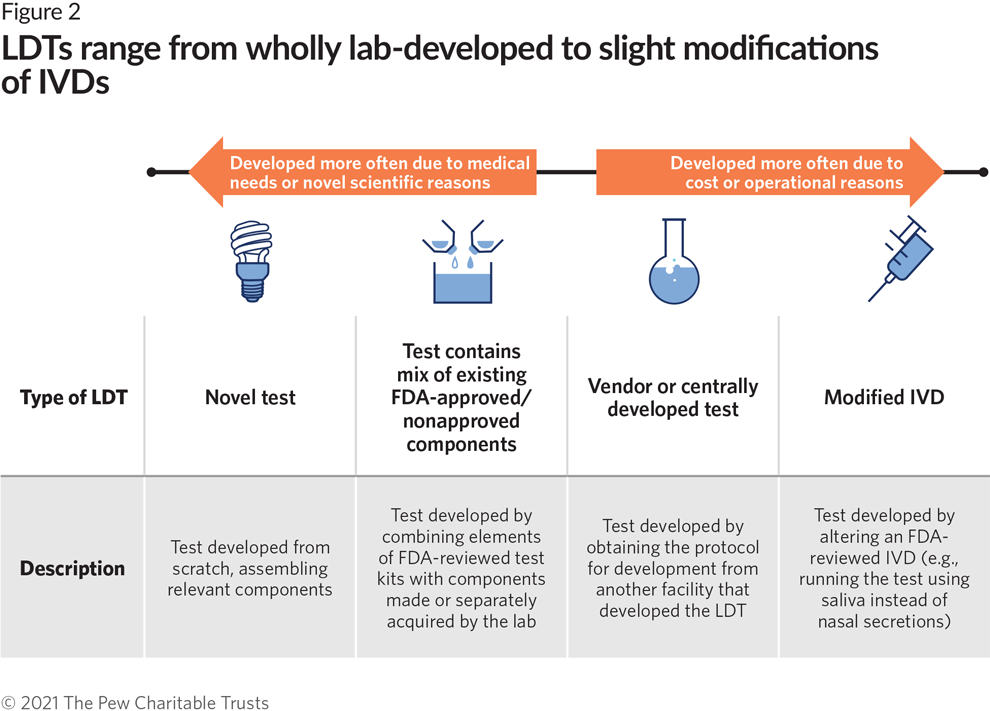
- Although some LDTs are developed from scratch to meet medical needs for which there are no IVDs, other labs create LDTs by modifying FDA-reviewed tests, in many cases to reduce operating costs. (See Figure 2.)
Real risks
Whether FDA approves them or not, all tests run the risk of delivering a false result. However, because labs are not required to publicly report adverse events associated with LDTs to a central authority, there is no comprehensive data quantifying the number and nature of incidents tied to inaccurate LDTs. According to FDA, inaccurate tests could cause patients to undergo unnecessary, costly, and risky treatment when tests return false-positive results. At other times, patients may fail to receive critical treatment when LDTs yield false-negative results.1
Some categories of tests illustrate just how little oversight there is for even widely marketed LDTs and how risky inaccurate test results can be when patients are relying on their results to guide medical decisions around everything from pregnancy to cancer treatment.2
- Noninvasive prenatal testing is a method of determining the risk that a fetus will be born with certain genetic abnormalities, such as Down, Edwards, and Patau syndromes. These tests help parents make critical decisions about a pregnancy and, as such, need to be carefully designed, administered, and marketed. Of the more than 40 noninvasive prenatal tests, all are LDTs3; none have been cleared or approved by FDA. Some companies advertise these tests for use in populations where their accuracy is less established, or to diagnose a broader range of conditions despite the limited evidence for those uses.4
- Risk: Expectant parents may be misled about the risk that a pregnancy has a chromosomal abnormality.
- Direct-to-consumer (DTC) genetic tests are, with relatively few exceptions, LDTs and not FDA-approved.5 One study estimated that more than 26 million people had taken a DTC genetic health or ancestry test as of January 2019, with the number expected to reach 100 million by the end of 2021.6 There is variable quality among manufacturers, however.7 One small study examined 49 patients who had taken a DTC genetic test and subsequently received follow-up testing. The authors found that 40% of the harmful variants reported back to those patients were false positives, indicating that the patients did not actually have those genetic variants.8
- Risk: These incorrect results can lead to stress and unnecessary medical procedures.
- Companion diagnostics guide the safe and effective use of a particular therapy and are often a key factor in treatment decisions, increasing the risks to patients if the results are incorrect. In some cases, after FDA approves one companion diagnostic, labs create follow-on versions of those tests that they claim can identify the same mutation.9 However, individual labs often have different approaches to analyzing samples. And some LDT developers claim to test for additional mutations that have not been adequately reviewed to predict drug response. 10
- Risk: The same patient may get different results depending on the LDT used11, receive ineffective therapies for their condition, or miss out on more beneficial ones. And many cancer treatments have serious side effects of their own, which can compound the harm for patients who receive an inappropriate therapy.12
Risk-based regulations balance safety and innovation
LDTs serve an important role in medicine and public health, but they must be held to the same standards for accuracy and reliability that apply to tests manufactured by device companies. This approach requires risk-based oversight from FDA and increased transparency from the entire diagnostics industry. To clarify confusion about FDA’s authority and strengthen its oversight, Congress should pass diagnostics reform legislation that:
- Requires developers of LDTs to register their tests with FDA and report adverse events related to their products.
- Allows FDA to require that higher-risk LDTs be reviewed for both analytical and clinical validity—both of which are key criteria for ensuring test accuracy, reliability, and usefulness—before they’re used on patients.
- Authorizes the agency to obtain information from LDT makers about the validity and performance of their tests once on the market.
- Appropriates funds to the agency that enable it to effectively oversee the entire diagnostics market, including developing regulations and guidance documents and conducting high-risk LDT reviews and facility inspections.
Endnotes
- U.S. Food and Drug Administration, “Laboratory Developed Tests,” last modified Sept. 27, 2018, https://www.fda.gov/medical-devices/in-vitro-diagnostics/laboratory-developed-tests.
- L. Richardson, “Clinical Lab Tests Need Stronger FDA Oversight to Improve Patient Safety,” The Pew Charitable Trusts, Jan. 11, 2021, https://www.pewtrusts.org/en/research-and-analysis/issue-briefs/2021/01/clinical-lab-tests-need-stronger-fda-oversight-to-improve-patient-safety
- M. Molteni, “How Much Prenatal Genetic Information Do You Actually Want?,” Wired, March 27, 2019, https://www.wired.com/story/how-we-reproduce-testing/
- Society for Maternal Fetal Medicine, “SMFM Statement: Maternal Serum Cell-Free DNA Screening in Low Risk Women,” accessed July 27, 2021, https://www.smfm.org/publications/157-smfm-statement-maternal-serum-cell-free-dna-screening-in-low-risk-women; R. Farrell et al., “Online Direct-to-Consumer Messages About Non-Invasive Prenatal Genetic Testing,” Reproductive Biomedicine & Society Online 10, no. 1 (2016): 88-97, https://doi.org/10.1016/j.rbms.2016.02.002.
- U.S. Food and Drug Administration, “Lists of Direct-to-Consumer Tests With Marketing Authorization,” last modified Dec. 20, 2019, https://www.fda.gov/medical-devices/in-vitro-diagnostics/direct-consumer-tests#list.
- A. Regalado, “More Than 26 Million People Have Taken an At-Home Ancestry Test,” MIT Technology Review, Feb. 11, 2019, https://www.technologyreview.com/s/612880/more-than-26-million-people-have-taken-an-at-home-ancestry-test/.
- S. Tandy-Connor et al., “False-Positive Results Released by Direct-to-Consumer Genetic Tests Highlight the Importance of Clinical Confirmation Testing for Appropriate Patient Care,” Genetics in Medicine 20 (2018): 1515-21, https://www.nature.com/articles/gim201838?mc_cid=b693215d3b&mc_eid=08a1c14744; A.D. Bowser, “Direct-to-Consumer Genetic Testing Fraught With Validity Concerns,” MDedge, April 16, 2019, https://www.mdedge.com/internalmedicine/article/199003/business-medicine/direct-consumer-genetic-testing-fraught-validity.
- Tandy-Connor et al., “False-Positive Results Released.”
- A. Towse and L.P. Garrison Jr., “Economic Incentives for Evidence Generation: Promoting an Efficient Path to Personalized Medicine,” Value Health 16, no. 6 (2013), https://doi.org/10.1016/j.jval.2013.06.003.
- J. Shuren, “Jeffrey Shuren, M.D., J.D., Director of the FDA's Center for Devices and Radiological Health and Janet Woodcock, M.D., Director of the FDA's Center for Drug Evaluation and Research on Agency’s Warning to Consumers About Genetic Tests That Claim to Predict Patients’ Responses to Specific Medications,” news release, Nov. 1, 2018, https://www.fda.gov/news-events/press-announcements/jeffrey-shuren-md-jd-director-fdas-center-devices-and-radiological-health-and-janet-woodcock-md.
- A. Stenzinger et al., “Tumor Mutational Burden Standardization Initiatives: Recommendations for Consistent Tumor Mutational Burden Assessment in Clinical Samples to Guide Immunotherapy Treatment Decisions,” Genes, Chromosomes & Cancer 58, no. 8 (2019): 578-88, https://pubmed.ncbi.nlm.nih.gov/30664300/.
- U.S. Food and Drug Administration, “In Vitro Companion Diagnostic Devices: Guidance for Industry and Food and Drug Administration Staff” (2014), https://www.fda.gov/media/81309/download.