New Therapy Shows Promise in Treating Metastatic Skin Cancers
2022 Pew-Stewart scholar working to advance melanoma treatment
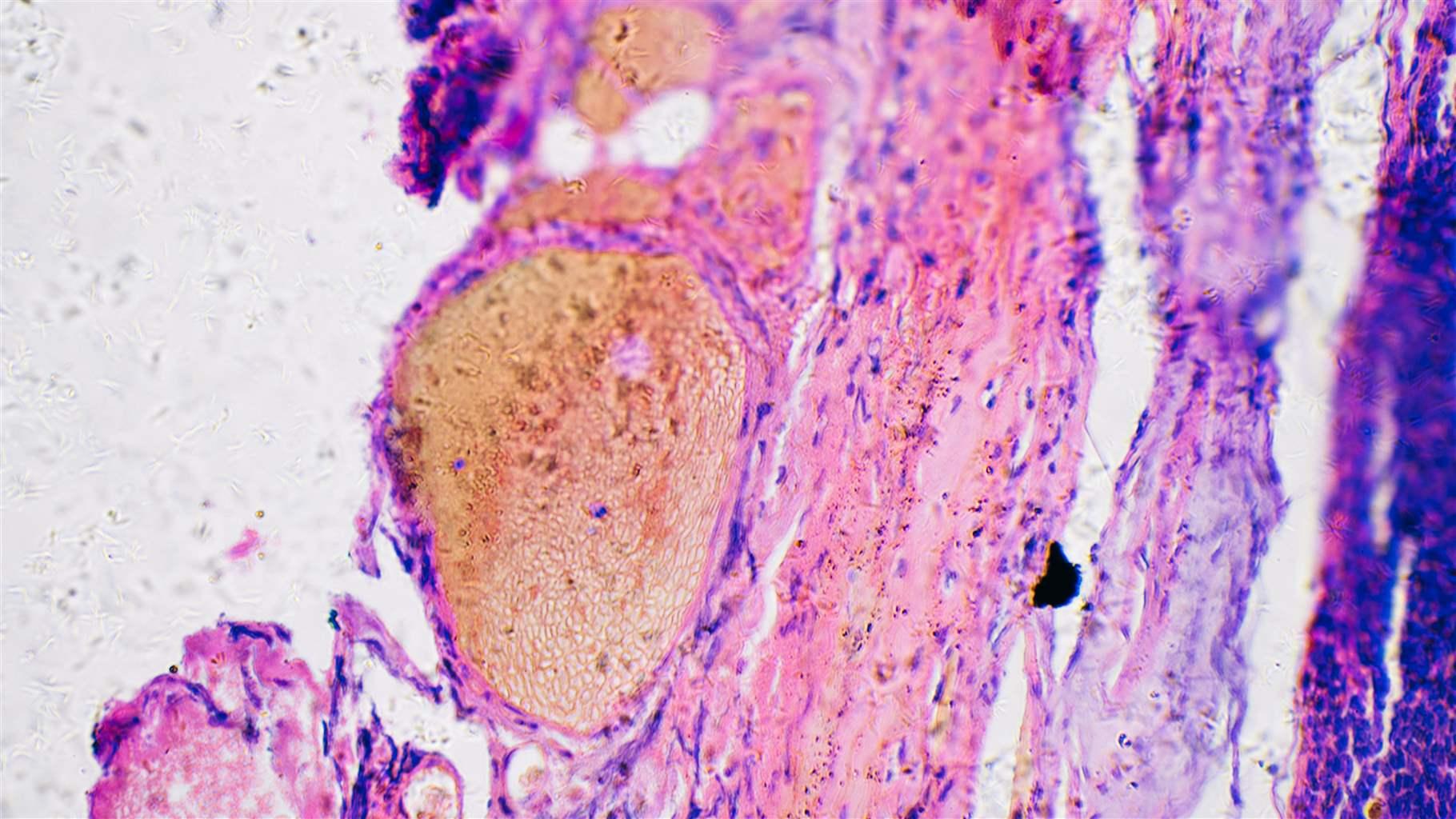
Skin cancer, one of the most common forms of cancer in the United States, often develops after prolonged exposure to the sun’s ultraviolet rays. Among the several types of skin cancer, melanoma—the rarest form—is most deadly if not caught early because of its ability to metastasize, or spread, undetected throughout the body.
This interview with 2022 Pew-Stewart scholar Alexander Huang, M.D., whose lab at the University of Pennsylvania is examining a promising new melanoma therapy, has been edited for length and clarity.
Q: What can you tell us about melanoma?
A: Melanoma develops when melanocytes—the cells that give skin its color—divide and grow uncontrollably. When caught early, melanoma can usually be treated, often by surgical excision. But because melanoma can metastasize to areas such as the lymph nodes, lungs, and brain before it’s discovered, patients often need more elaborate and invasive therapies to address the disease in its later stages.
Q: What’s the state of melanoma treatment today?
A: In 2009, when I first started in this field, patients with metastatic melanoma lived an average of nine months, and no treatments existed that could extend their life. Now, new therapies have transformed this outlook. Some are targeted therapies that take aim at specific mutations in the tumor directly. Other treatments known as immunotherapies, which activate a patient’s immune system against the tumor, have also shown real promise. My lab is exploring checkpoint inhibitors—a type of immunotherapy that targets immune checkpoints, which are proteins that serve as brakes to keep the body from destroying healthy cells. Blocking immune checkpoints allows the immune system to mount an unrestricted attack on a tumor.
Q: Which of these new treatments is most effective?
A: We have checkpoint inhibitors that target two specific immune checkpoint proteins (CTLA-4 and PD-1). When used together as combination treatment, half of the patients with metastatic melanoma who received this immunotherapy are alive at least five years from diagnosis.
Q: That’s great news. Are there any downsides?
A: Yes. This is a major advance in the field, but patients receiving this treatment have also experienced adverse side effects associated with toxicity.
Q: Can you elaborate on toxicity?
A: A major challenge with treating melanoma is balancing a drug’s effectiveness against cancer with its toxic effects on healthy cells. Although checkpoint inhibitor therapy is very effective, it comes with a high degree of toxicity, which can lead to serious inflammatory side effects. Scientists need to understand how to increase the effectiveness of the treatment while decreasing these adverse side effects.
One of the newest and promising checkpoint inhibitors in clinical trials target the proteins LAG-3 and PD-1, which have the potential for a similar degree of efficacy with significantly lower toxicity.
Q: What else do scientists need to understand to improve treatment?
A: We’re also working to better understand treatment needs in earlier stages of the disease, such as whether patients need additional treatments after surgery. We give many patients checkpoint inhibitor therapy after removing melanoma from the skin and/or lymph nodes to decrease the likelihood of recurrence. However, in many cases, treatment with immunotherapy may be unwarranted—since these patients have already been cured with surgery. We need to be able to identify which patients can forgo further treatments—thus limiting their exposure to potential toxicity—and which patients still need those treatments.
Q: Is that where your work comes in?
A: My lab is studying the combination checkpoint inhibitor therapy that targets the proteins LAG-3 and PD-1. Specifically, we’re using cutting-edge approaches to understand the changes that happen to immune cells during immunotherapy, and how resistance to treatment develops. In other words, when and why does the treatment stop working? For example, how large, or how durable, are the immune responses? Which immune cells are targeted? Which proteins and cellular pathways are turned on or off in these immune cells? Which of these proteins and cellular pathways contribute to treatment efficacy, and which ones contribute to toxicity?
Q: What impact could these findings have on treating melanoma?
A: Understanding the patterns for immune responses generated by immunotherapies will help us learn which treatments are more effective and which treatments have more side effects. Ultimately, this could help us engineer a safer and more successful treatment for patients with metastatic melanoma.
Q: What’s the end goal?
A: Today, we have genetic tests for profiling hundreds of tumor mutations and identifying targeted therapeutic approaches for each individual. My long-term goal is to develop a test that will allow us to profile dozens of immune mechanisms of response, resistance, and toxicity, which can help to guide precise immunotherapies for individual patients.
Q: How will funding from the Pew-Stewart Scholars Program for Cancer Research help support your work?
A: The funding will help establish our “Precision Immune Profiling Pipeline,” where we link cutting-edge technologies to computational systems such as machine learning algorithms. We’ll apply this pipeline to clinical trials across the Abramson Cancer Center at the University of Pennsylvania, to understand what determines whether a patient has a good clinical outcome and/or drug toxicity.
I’m excited to be part of the Pew community now, especially because of the people I’ll get to meet and the relationships that will develop. That’s what makes research so rewarding—the colleagues and mentors, and mentees, and the lifelong bonds that result.