New National Action Plan for Combating Antibiotic-Resistant Bacteria Lacks Essential Details
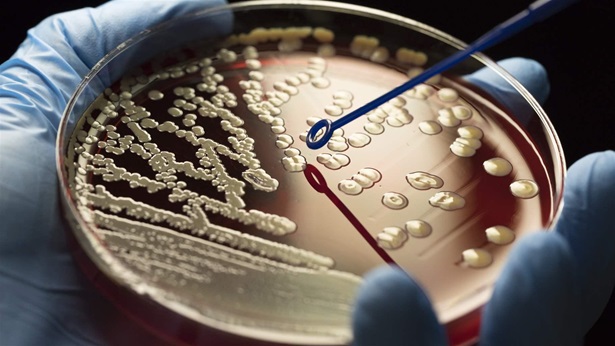
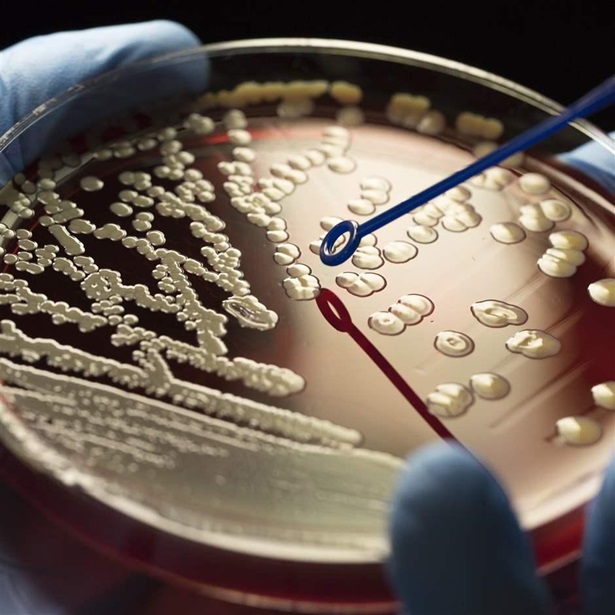
Update underscores growing threat posed by superbugs but represents a missed opportunity
The federal government recently reinforced the importance of the fight against superbugs when it released an updated National Action Plan for Combating Antibiotic-Resistant Bacteria, but the guidance to agencies lacks details on specific policies and on ways to achieve key priorities.
The October update of the plan first published in 2015 calls for continued work in many essential areas, identified earlier by Pew and others, to fix the broken antibiotics market and promote antibiotic stewardship. The document highlights the need to implement policies that stimulate development of urgently needed drugs, strengthen the country’s capacity to track antibiotic resistance and use, and improve antibiotic use in humans and animals. Still, the 2020 update would have benefited from more specifics on the economics of essential antibiotic development and what steps should be taken.
For example, the new action plan lacks a mechanism to ensure measurable progress in the implementation of a package of economic incentives to boost investment in antibiotic discovery and development and to create a sustainable market for these lifesaving drugs. To help jump-start the development of new antibiotics, lawmakers have already introduced bipartisan measures, such as the Pioneering Antimicrobial Subscriptions To End Up Surging Resistance (PASTEUR) Act of 2020 and the Developing an Innovative Strategy for Antimicrobial Resistant Microorganisms (DISARM) Act of 2019. The recent update, however, includes no mention of such approaches.
The plan does call for the continuation of existing government efforts to stimulate antibiotic innovation, including adjustments by the Centers for Medicare & Medicaid Services to antibiotic reimbursement as well as initiatives from the Biomedical Advanced Research and Development Authority to purchase antibiotics for national security purposes. However, these efforts are not sufficient to repair the antibiotic market.
Much like the 2015 national action plan, the update focuses on supporting antibiotic discovery and development rather than enacting incentives to adequately address the troubled market. Additionally, the new plan does not mention the need to improve the sharing of antibiotic research data, which experts agree is essential for catalyzing urgently needed antibiotic discovery.
In addition, the government and health care stakeholders must improve the capacity to monitor antibiotic use and resistance so they can quickly identify and combat superbug outbreaks. Effective stewardship policies for reducing inappropriate prescribing also are essential. Increasing the number of hospitals reporting antibiotic use and resistance data to the Centers for Disease Control and Prevention’s National Healthcare Safety Network would represent fundamental progress in this arena. The 2020 plan sets a series of goals for hospital reporting but lacks specific strategies and policies to reach those goals by 2025.
Any national strategy should also promote appropriate antibiotic use in humans and food-producing animals to combat antibiotic-resistant bacteria. Research shows that the more often antibiotics are used, the less effective they become. However, the updated plan falls short on both fronts.
In antibiotic use in human medicine, Pew strongly supports the prioritization of improving antibiotic prescribing in doctor’s offices and other outpatient health care settings. Research from CDC and Pew shows that 1 in 3 outpatient antibiotic prescriptions is unnecessary, which puts patients needlessly at risk and accelerates the emergence of resistance. Although the 2020 national action plan calls for a decrease in antibiotic prescribing in outpatient settings and improved timelines for outpatient antibiotic use reporting, it does not include specific targets or interventions for developing antibiotic stewardship in these settings. Such programs help to ensure that these drugs are used appropriately and only when necessary.
Regarding the judicious antibiotic use in farm animals, the plan includes no direct reference to the Food and Drug Administration’s five-year plan to improve antibiotic stewardship in these animals. It also lacks specifics on how and when the agency will collect and publicly share important new information about antibiotic use in animals. For example, there is no mention of when or how FDA will start adjusting antibiotic sales data based on the size of animal populations—a step that that would provide valuable context to the meager existing information on agricultural antibiotic use. The agency has committed to doing this but has yet to take any concrete action.
In the same vein, the plan does not include specifics or timelines for establishing evidence-based durations of use for all medically important antibiotics given to the animals and other steps to ensure that these drugs are used judiciously. Currently, many antibiotics can be given to animals for weeks, months, or even indefinitely. Failure to address this problem in the new action plan is a clear omission.
The updated plan signals that the fight against antibiotic resistance is—and should remain—a national priority, but a lack of clear benchmarks, metrics, and strategies for achieving its stated goals is a missed opportunity. Pew encourages federal agencies to take steps to improve this and future national action plans and looks forward to coordinating with policymakers and other stakeholders to drive meaningful progress on the real and growing threat posed by superbugs.
David Hyun, M.D., works on The Pew Charitable Trusts’ antibiotic resistance project.