Antibiotics Are Overprescribed in Urgent Care
New study adds to body of research on use of these drugs in the U.S., shows less overuse in retail
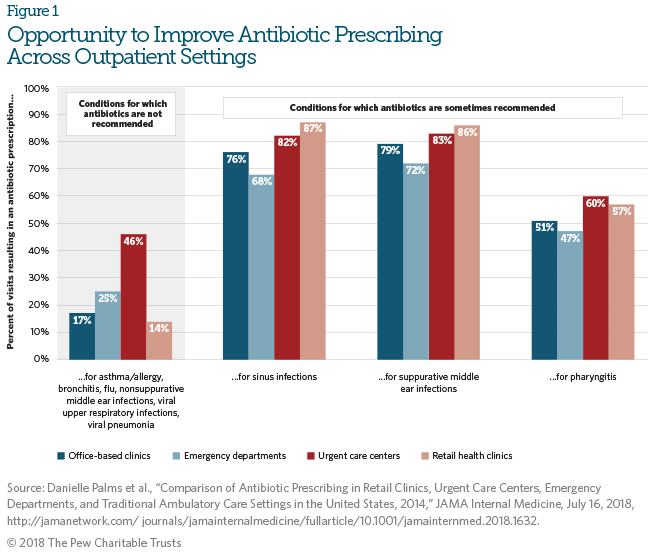
Patients seen at urgent care centers for common conditions such as asthma, the flu, and the common cold are more likely to receive antibiotics unnecessarily, compared with patients treated for the same illnesses at other types of health care facilities. In fact, nearly half (46 percent) of patients in urgent care centers who were diagnosed with one of the acute respiratory conditions for which antibiotics are neither recommended nor effective received an antibiotic prescription anyway. In retail health clinics, just 14 percent of patients did. This information comes from new research by The Pew Charitable Trusts and the Centers for Disease Control and Prevention (CDC) that was recently published in JAMA Internal Medicine. The research looks at antibiotic use in retail health clinics (located within businesses such as pharmacies and grocery stores) and urgent care centers, which are typically stand-alone facilities where patients seek immediate and unscheduled care. Both play a large role in providing outpatient care in the U.S.
The study also showed that health care professionals at these two types of facilities prescribe antibiotics at more comparable rates in situations where antibiotics are sometimes but not always indicated: for diagnoses such as sinus infections, suppurative middle ear infections (identified by the presence of pus), and pharyngitis (inflammation of the throat). (See chart below.) Although some of this prescribing is appropriate, inappropriate prescribing is also likely for these conditions. For example, the use of antibiotics does not alter the course of the illness for some of these conditions, and others can be caused by viruses, which should not be treated with antibiotics.
This new information is part of an ongoing collaboration between Pew and CDC to better understand and improve antibiotic prescribing in the U.S., which is key to slowing the spread of antibiotic-resistant superbugs. The findings build on previous research led by Pew and CDC using different data sources, which showed that:
- High amounts of unnecessary prescribing persist across various outpatient settings in the U.S.
- Acute respiratory infections—such as common colds, the flu, and bronchitis—are the main source of inappropriate prescribing in outpatient settings, accounting for the largest proportion of unnecessary use.
- Patients with acute respiratory infections often do not receive the recommended treatment.
The growing body of research in this area will help inform efforts to improve antibiotic use across the country and drive continued progress toward the national target of cutting inappropriate outpatient antibiotic prescriptions in half by 2020. Effective stewardship across all outpatient settings—including retail health clinics and urgent care centers—is essential for such progress. It could also help reduce unnecessary prescriptions written because of patient pressure felt by doctors, who may fear losing patients to competitors or may believe it is futile to refuse prescribing an antibiotic if patients can simply go to another doctor to get a prescription.
Knowing that all antibiotic use contributes to the emergence of resistance, Pew and the CDC will conduct a nationwide assessment of antibiotic prescribing in inpatient health care settings, such as hospitals and long-term care facilities. These efforts will help policymakers, health care professionals, researchers, and other stakeholders ensure that antibiotics are used appropriately, and only when necessary.
David Hyun, M.D., and Rachel Zetts work on Pew’s antibiotic resistance project.