Federal Dental Health Strategy
Strong workforce, school sealant programs
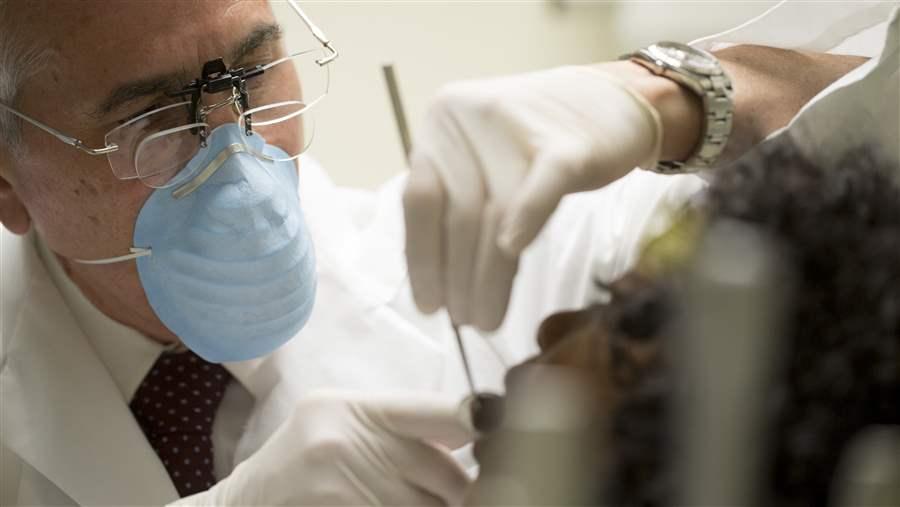 © The Pew Charitable Trusts
© The Pew Charitable TrustsThe U.S. Public Health Service has released a plan listing strategies to improve access to care and address disparities in dental health.
A new federal government plan, which lists partnerships and strategies needed to address persistent dental health disparities in the U.S., states that access to care is one of the greatest unmet oral health needs in the nation. The proposal serves as a call to action for federal agencies, the private sector, and other partners to reduce this and other barriers to improved dental health for the underserved.
Poor oral health disproportionately affects low-income families, people living in dentist shortage and rural areas, and communities of color. In his forward to the plan, Surgeon General Vivek Murthy acknowledges that these inequalities persist 15 years after the first surgeon general’s report on the dental health of Americans spotlighted these problems. For example, one-quarter of prekindergarten-age children living in households below the federal poverty level have untreated tooth decay, compared with about 1 in 10 children living above the line.1
The plan focuses on five goals to improve dental health and increase access to care:
- Integrate oral health with primary health care.
- Prevent disease and promote dental health.
- Increase access to care and eliminate disparities.
- Increase the dissemination of information and improve health literacy.
- Advance dental health in public policy and research.
In particular, the plan cites dental sealants as an effective strategy to help prevent decay, and it calls on stakeholders to promote school-based sealant programs that target low-income children. Dental sealants are plastic coatings placed on the chewing surfaces of teeth and cost about one-third as much as a filling, saving patients, families, and states money.2 Programs that make this treatment available in schools to underserved populations can reduce decay by 60 percent.3 However, a 2015 Pew report found that the majority of states (39) plus the District of Columbia do not have sealant programs in most of their high-need schools. A number of organizations, including Pew, are conducting research to better understand the barriers to expanding these programs and to identify ways to improve their efficiency.
The plan also calls for strengthening the dental health workforce and expanding the capabilities of existing providers. Allowing dentists to hire dental therapists—midlevel providers who are similar to physician assistants on medical teams and provide preventive and routine restorative care, such as filling cavities—is one way to address the workforce shortage and improve access to care. These practitioners already work in Alaska and Minnesota, where they are helping dentists to see more patients and increase revenue.4 Maine authorized dental therapy in 2014 and is now working to implement the law. Oregon also recently approved a pilot program allowing two Native American tribes to hire dental therapists in clinics and centers. At least 10 other states are considering laws and other proposals to enable dentists to incorporate dental therapists into their teams.
The federal plan highlights community and clinical strategies that policymakers know eliminate disparities in dental health. It also acknowledges that those approaches aren’t being used to their fullest potential. Dental health inequities cannot be overcome without continued action.
Jane Koppelman directs research on children’s dental policy at The Pew Charitable Trusts.
Endnotes
- Bruce A. Dye et al., “Oral Health Disparities as Determined by Selected Healthy People 2020 Oral Health Objectives for the United States, 2009–2010,” National Center for Health Statistics, NCHS Data Brief no. 104 (2012), http://www.cdc.gov/nchs/data/databriefs/db104.htm.
- American Dental Association, Health Policy Institute, “2013 Survey of Dental Fees” (2014). The national median charge among general practice dentists for a sealant (procedure code D1351) is $48, and the national median charge for a one-surface posterior composite filling (procedure code D2391) is $160.
- Benedict I. Truman et al., “Reviews of Evidence on Interventions to Prevent Dental Caries, Oral and Pharyngeal Cancers, and Sports-Related Craniofacial Injuries,” American Journal of Preventive Medicine 23 (2002): 21–54, http://www.thecommunityguide.org/oral/oral-ajpm-ev-rev.pdf.
- The Pew Charitable Trusts, “Expanding the Dental Team: Increasing Access to Care in Public Settings” (June 2014), http://www.pewtrusts.org/~/media/assets/2014/06/27/expanding_dental_case_ studies_report.pdf; and The Pew Charitable Trusts, “Expanding the Dental Team: Studies of Two Private Practices” (February 2014) http://www.pewtrusts.org/~/media/legacy/uploadedfiles/pcs_assets/2014/ expandingdentalteamreportpdf.pdf.







